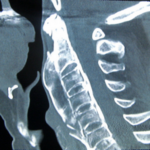
Fracture or overload reaction, overload fracture (fatigue fracture), stress reaction, continuous load
Key words: fracture or overload reaction, predisposition to acute or chronic fracture, repeated minor injuries, march fracture, stress reaction, “insufficiency fracture”, remodelling zone, disproportion between load and load-bearing capacity, overloading of the supporting apparatus, skeletal weakness, lat: “locus minoris resistentiae”, fatigue fracture on pre-damaged bone, osteomalacia, vitamin D deficiency, osteoporosis,
calcaneus, distal tibia, lateral tibial plateau, Os metatarsale,
growing or mature bone, Reconstruction zone, repair processes, growth plate, soft tissue oedema, metaphysis, aseptic necrosis, Scheuermann’s disease, Köhler’s disease I and II, Perthes’ disease, lunate malacia, Schlatter’s disease, apophysitis, Achilles tendon swelling.
Lack of self-awareness, lack of personal responsibility, overweight, second half of life, endorphin release, gentle therapy, scintigraphy, NMR, MRI, classic spin echo sequence, inversion recovery: STIR sequences, T1, T2 sequence, methods of fat saturation, gradient echo T2*, “T1-KM saturated”, distribution of iv gadolinium- DTPA, , methaemoglobin, pathological signal, medullary oedema, hyperaemia, contrast agent distribution, skeletal scintigraphy.
The common thread of this work is a comparison of different forms of osseous insufficiency, regardless of where they occur.
Chapters I – III do not strictly follow the body regions.
I (knee joint, lower leg, calcaneus)1- 18
II (hip joint, thigh and pelvis) 19 – 39
III ( differential diagnosis, growth plates, knee, foot, hand, elbow, shoulder, spine, sacrum-iliac bone, ribs, sternum) 40 – 63
After this cursory table of contents comes the instructions for use. Please, dear reader, do not go to these desired chapters (I -III) before you have seen the next pages, the introductory text . –
The following picture, or rather the pictures that you see when “scrolling through”, are not yet part of the actual article. They are intended to arouse interest and document the diversity. Everything seems very different, and yet the cause is almost the same; a mismatch between stress and resilience! This is a message that could be very irritating to some people, even those with experience.
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
(14.5.24)This 6 point scheme should be used for almost all of the approx. 60 cases of the disease! It is explained in more detail below.
I try to shed light on the differences and similarities between different forms of “stress on the bone”.
By the way: Soft tissues (muscles and tendons) are also susceptible to injury (trauma). There are also acute or chronic traumas.
I show isolated cases of illness that “at first glance” have nothing to do with stress: inflammation or neoplasms (cancer). But these diseases can also be “secondarily” susceptible to overload; susceptible because the bone has somehow become too weak to withstand even normal stress.
Our question involves many and very different terms! We are trying to do something that has rarely been attempted before, to organise the chaos. In this respect, the work starts with the claim of wanting to achieve a pioneering feat. Fortunately, it turns out
- that there are many simplifications,
- that you can understand many things and don’t have to memorise them at all!
Our bones can take a lot:
- One-off high loads (jump from height, rollover, rollover)
- But also with many small loads: constant stress
At a certain level of stress, it becomes too much:
- Both with monostress: the support system, the bone, no longer holds up, breaks = fracture. This is called an “acute trauma“.
- If the many small stresses become “too much” – this is called “chronic trauma” – the bone reacts with an overload reaction or even a stress fracture.
The most important tool for differentiating between 1 and 2 is the history.
Would it also be possible to tell from the X-ray whether it was an acute or a chronic trauma?
The bone reacts to different forms of stress, but it needs time to do so. In acute trauma, it does not have time to heal.
In the second, chronic form, healing begins during the damage (noxious agent). So the permanent stresses, the many small “stresses”, continue at the same time as the attempts at reparation. Why is there such nonsense, such a coexistence of healing and continued damage? The overload is not realised (by the person) or its signals are suppressed.
In the following article (02.), my co-author and I describe a “psychodynamic model”: Toughness, masculinity, pride, will are the driving forces behind a suppression of body signals. People are under the mistaken impression that they have to show toughness, that they have to “get through it”. The messages from the body, its signals, are not recognised and/or not understood.
What can be done?
- Recognise the mechanisms!
- Stop what is harmful!
- Giving healing a chance.
- Gain insight into the flawed nature of a training concept.
- Totally restructure and fundamentally improve your training programme.
A tough will can be stronger than your bones can handle. – How have world-class athletes managed to endure high to the highest demands for a long time, and even increase them?
The training of world-class athletes is like juggling with eggs: Too little and the competition is ahead. Too much and the damage is done and everything is set back. Many fall by the wayside. At some point, pain and functional limitations become apparent. Now there is a risk of causing serious damage. He who goes far wins, but not too far.
You have to admit, those who actually reach world class are a selection of stress resilience and they have been very lucky.
Being a world-class athlete actually (only) means having good resistance to overload damage, remaining sensitive to the limits of what is reasonable and probably being lucky in this game of vabanque.
If you don’t belong to a gifted selection, you don’t have to “run the Zugspitze”. They don’t have to run a marathon. He has to understand that he has limits. And they must learn to recognise where are the limits of my resilience.
With destructive intent, a person can inflict both acute and chronic injuries.
The vulnerability of the bony supporting tissue is very difficult to assess.
The musculature is easier to assess, it is more sensitive and reacts with “sore muscles”; its signals are faster, so that more serious damage is more likely to be avoided. This would be muscle tears and haemorrhage (without acute trauma, only through constantly repeated small noxious agents).
This delay in the muscle reaction is shorter than on bones, but still long enough to cause some people to be agonised: larger muscle groups can be put out of action due to pain.
If the muscle soreness started immediately, most people would stop sooner. It is only this silent period of time combined with psychodynamic peculiarities that allows us to ramp up the noxious agent to such an extent that it can become very unpleasant afterwards.
Intense muscle soreness means a setback in training. The gap is difficult to make up. The person responsible for training has made a mistake.
Another example to help you understand the support system, mistakes during training: Hiking boots squeeze and subject a toenail to many small pressures and shear forces. At first the nail hurts, its bed is reddened and swollen. Finally, a haematoma forms under the toenail. The nail may come off. Fortunately, the damage is so well visible. Fortunately, the tortured toe also makes itself known relatively early on and lets even the bravest person realise that the whole thing is a typical chronic trauma. If such a trauma is on the bone, it is much more hidden from view and insight. Then there are regularly these nonsensical referral diagnoses: “to rule out tumour”, “osteomyelitis”, “venous thrombosis”. The referrer doesn’t dare to say: “Probably mismatch between stress and resilience He didn’t understand this connection!
An example from another organ system that helps us to understand the support system: sensible exposure versus excessive exposure. If you want to get a tan, you have to sunbathe, but you should avoid sunburn. In the worst case, the person is ill for days. It is painful, costly and unhealthy. So only get enough sun to avoid sunburn; otherwise the plan to “tan” is wrong. – (Basically, one should be careful with sun exposure).
Back to the “bone”.
Unfortunately, “acute trauma – chronic trauma” is not the only difference:
Both can namely affect healthy bone tissue – or – diseased, i.e. pre-damaged bone tissue.
It is quite conceivable that the disease of the bone affects not only the strength, but many other properties. There is a complex metabolism that is not only characterised by fracture resistance.
After all, there is a third, essential difference, namely whether it is an
adult or a growing human.
The sensitivity of the bone and also the weak point are different in different phases of growth. Growth takes place along so-called growth zones. These regions – with their mysterious and marvellous abilities – are particularly sensitive.
In every case of bone injury, I suggest applying the following scheme and will try it out on about 60 patients. It contains the above-mentioned 3 alternatives.
I will always list all 3 alternatives, but only mark the applicable with red:
| Acute trauma in growth healthy bones |
| Chronic trauma Outgrown diseased bone |
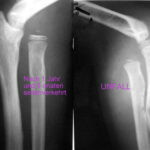
One of the three applies, either above or below. The one that applies is RED! Be careful, the colouring is somewhat atypical! Above is an example: a healthy adult athlete who has broken his radius in a fall. Acute – healthy – adult .
However, there are other constellations of osseous insufficiency, a total of 8!
I. knee joint,lower leg, calcaneus 01 – 18
01 / Acute trauma of an adult with overall healthy bone

| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
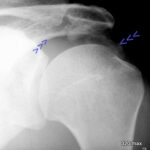
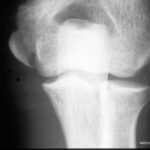
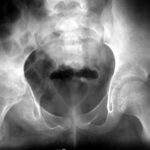
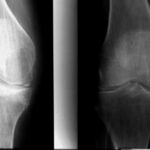
The 63-year-old patient fell on the cellar stairs. She walked 300 metres to the clinic. Slight spontaneous pain. Moderate compression pain. As she described it to me, she did not fall on her knee, but twisted it with strong pressure on the inside of the knee.
I have slight doubts as to whether our patient has a healthy bone or already has minor osteoporosis. According to QCT, it is a: Still healthy bone.
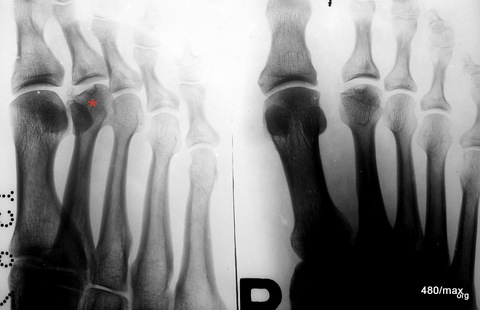
In the X-ray image, it is interesting to note that the plateau of the tibial plateau and the very close cancellous bone (the spongy interior of the bone) are affected. Bone balls are pushed together and thus compacted (lighter in colour than normal!).
A nice experiment on the compaction of spongy material was shown in the article x y. – An experiment from “Pleura I” shows why the often wafer-thin compacta (the outer lamella of the bone) can be seen so beautifully in X-rays.
The treatment was conservative. The patient kept to the house and avoided stairs; she was symptom-free after 4 weeks.
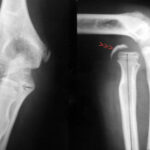
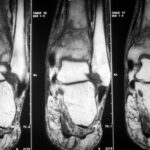
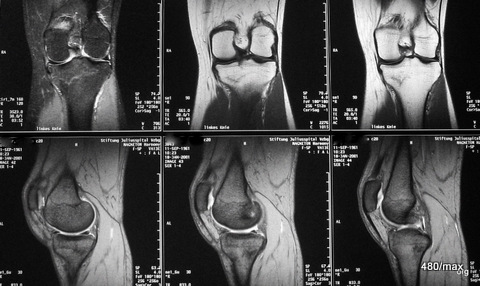
02 / Stress fracture (= overload fracture) in the tibial plateau during/after harvesting
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
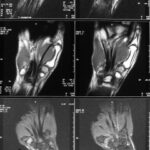
02. 43-year-old patient; due to good weather, 6 days of continuous work during the harvest: drove combine harvester, shovelled, climbed on machines many times.
Pain, 3 days after the work was finished.
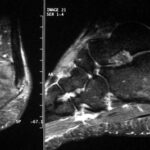
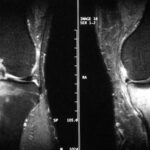
This time we show MR images. – What distinguishes this patient from case 1? In addition to the history, the location of the pathological change is different: although the knee joint is also affected, the change is not located in the plateau of the tibial plateau, but in the middle of it!
With regard to the MR signs, compare with article 02 “Osseous insufficiency II”: Fracture zone and surrounding oedema.
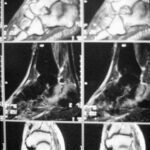
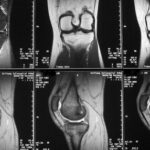
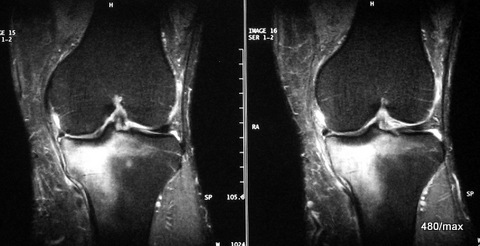
03 a / Overload reaction in the medial tibial head MR: STIR
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
03. 48-year-old man, stood in for family and friends on the building site. Loaded and hauled a lot of wood.
It is very plausible that he overloaded himself. When the pain got worse, he finally had to stop after all. The clinical findings were not impressive.
MR: No collapse of the tibial plateau, i.e. no fracture zone in the centre of the tibial plateau, but only diffuse oedema. This is a reaction in the bone marrow with increased fluid (some of the abundant fat must give way in the narrow conditions in the medullary cavity). This could have developed into a classic stress fracture (as in 02).
“Medial” is towards the centre, as opposed to “lateral”, which means “to the side”.
Which sequence is used for the next sequence (in the same patient)?
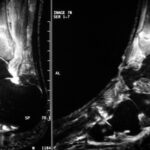
03 b / (same case) Tibial head overload reaction. MR: Now T1 instead of the “STIR”
Here at T1, the water is dark (almost everything pathological is accompanied by an increase in water). Fat is very light in colour. (This makes for a beautiful anatomy).

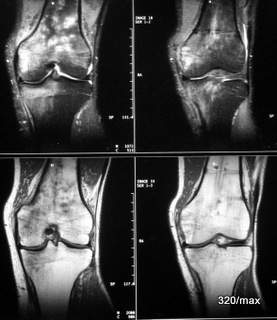
04 / New case of disease: intramedullary nail, now acute stress reaction in the tibia + femur area
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
04. history: fall from the roof. Femur fracture. The osteosynthesis (operation on the fracture with intramedullary nail of the femur) was 2 years ago, the removal of the intramedullary nail 8 weeks ago.
Even then – after the osteosynthesis – the patient could not be stopped from planting a garden. Everything went well.
Recently, after the nail was removed, he was symptom-free after a few days and fully active in building the house again. He reports that he touched the spit in the bucket faster than the younger employees could install it. Then he started to feel pain and was forced to stop.
MR: Patchy bone marrow oedema in the tibia and femur.
Since both bones (tibia + femur) are affected, one could think of an“activated arthrosis“. ? But the oedema is not sufficiently related to the joint region; there are also no indications in the history and on the images of pre-existing osteoarthritis.
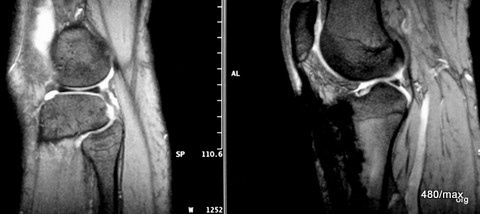
05 a / Intramedullary nail of the tibia with artefacts due to metal abrasion. Incorrect loading in the knee with small medullary oedema in the medial femoral condyle. Probably caused by incorrect loading with “heel spur” on the other side.
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
05a. MR images: proton weighted on the left, gradient echo on the right;
the latter is very sensitive to fine iron particles and therefore susceptible to artefacts. The image would also fit into the article “Artefacts (iatrogenic)”. Only slight knee joint effusion.
I am the patient myself. I suffered a spiral fracture of the tibia 35 years ago while cornering on roller skates. There is no definite connection between this and the intramedullary nail that has since been removed. It started with pain in the other foot with a classic heel spur (not shown here). It seems classic to me because parts of the tendon plate of the sole of the foot, which is called the plantar aponeurosis, and also parts of the calcaneus were affected. It was not just a bony attachment of this tendon plate that was altered! In the era before MR, we liked to reduce the term “heel spur” to what you see on the X-ray. Now it is increasingly recognised that it is a disease of both bone and soft tissue.
The main cause is incorrect loading/overloading. When the severe pain in the heel bone and sole of the foot appeared, I started to put “incorrect” strain on the knee on the opposite side until it also reacted “offended”.
05 b / (same case) MR slice images in a second plane.
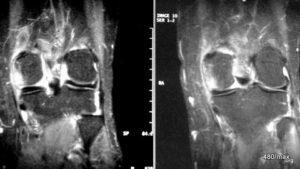
MR slice images of a second plane. All “water” is bright in this STIR: small oedema in the femoral condyle. The above-mentioned very small medullary oedema is an expression of the incorrect loading.
There are too few typical signs of osteoarthritis for “activated osteoarthritis”. I therefore assume a (not pronounced) stress reaction.
The symptoms soon improved, even with rest. The symptoms in the foot on the opposite side also improved.
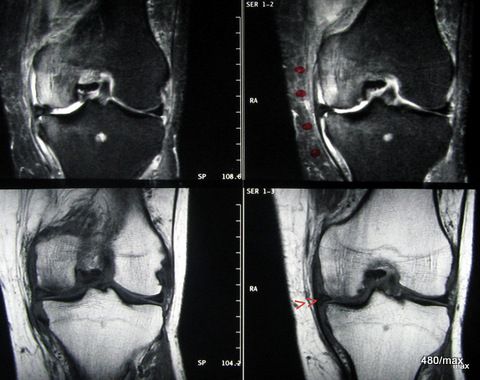
06 / 65-year-old doctor, osteoarthritis, overloading when climbing stairs, pain.
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
06. 65-year-old doctor. He was filling in at a practice that extends over two floors. Untrained, he had to be constantly on the move between the two floors for two working weeks. Osteoarthritis in his knee joint has been known for 3 years. He already had pain in the left knee joint on the medial side after the end of the operation.
MR top: STIR lateral, bottom T1; fatty tissue in STIR typically strongly suppressed. If the musculature is much lighter in colour than fatty tissue, this is typical for normal tissue in STIR. This is why the sequence is so well suited for the sensitive detection of any form of pathological fluid increase. Displacement of the medial meniscus and small joint effusion. Oedema in the medial femoral condyle and also in the medial tibial plateau. As with almost all overuse injuries, this reaction spreads to the neighbouring tissues, which are functionally involved: medial ligamentous apparatus and the overlying soft tissue.
With this history and the findings: activated osteoarthritis.
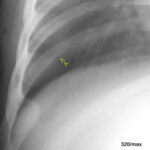
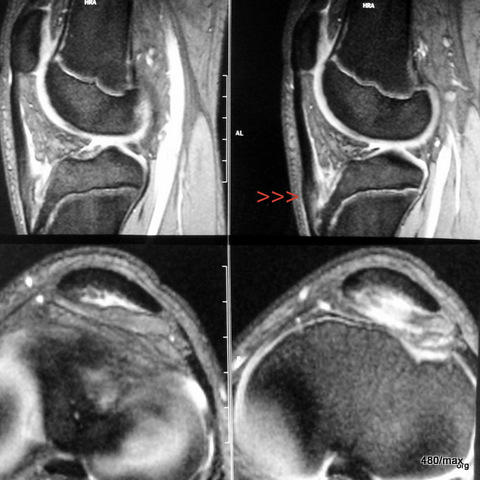
07 / Athlete. Tendinitis of the patellar tendon, MR: two images in T2 gradient echo
| Akutes Trauma | im Wachstum | gesunder Kn.+ Sehne |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
07. 21-year-old “jumper”, English is didactically favourable, because in the Anglo-American language area careful attention was paid to sports injuries. (see the story of the discovery of the “shin splint”). Here in Central Europe, people were somewhat slow to realise the connections.
Preceded by intensive training for the long jump.
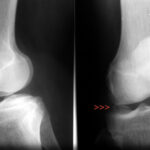
The swelling and fluid deposits (red arrowheads) in the patellar tendon directly at the origin from the patella (kneecap) are clearly visible.
The images below show the transverse view at the level of the knee joint space and just below it at the level of the tibial plateau.
08 / Other athlete, also “jumper”; oedema of the patellar tendon near the patella; MR: T2 left and T1 right

| Akutes Trauma | im Wachstum | gesunder Kn.+ Sehne |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
08. 21-year-old track and field athlete. Promising young talent. Preceded by hard training for the triple jump. Circumscribed pain – aggravated with exertion – in the kneecap and below it.
MR: left-sided STIR: fatty tissue strongly suppressed compared to spin echo T2. Right-sided T1. The swelling and fluid accumulation (red arrowheads) in the patellar tendon directly at its origin from the kneecap (patella) is clearly visible.
09 / 56 year old man, incorrect load due to obesity + excessive and unusual work during house construction.
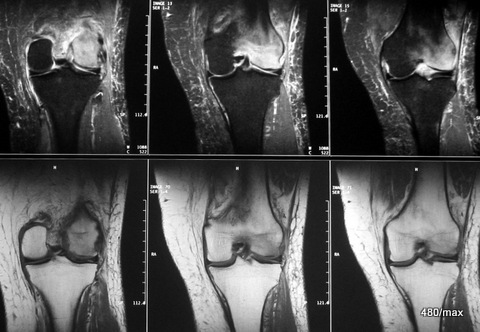
| Akutes Trauma | im Wachstum | gesunder Kn.+ Sehne |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
MR top: STIR, fat strongly suppressed; this is why the oedema is visible in the entire lateral femoral condyle.
The images below show T1: The light-coloured fatty tissue dominates the image. Only the lateral femoral condyle is darker: here the fat has been displaced by the inflammatory reaction.
The neighbouring soft tissue also reacts with fluid retention.
10 a / Haemophiliac joint in a child. X-ray of both knee joints in 2 planes. Projection from the front (a-p). Further down (10b): seen from the side.

| Akutes Trauma | im Wachstum | gesunder Kn.+ Sehne |
| Chronisches Trauma | Ausgewachsen | sekundär.kr.Knochen |
10 b
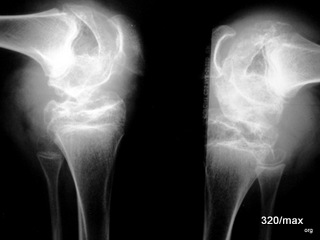
The coagulation system of this young person has a disease that spreads to the bone and damages it. The continuous haemorrhaging into the joint, even with the slightest injury, causes ongoing damage to the cartilage, the bone close to the joint and the growth plates. In the case of the sum of many small traumas, one can probably speak of chronic trauma. The many minor injuries would be harmless if they did not affect a bone that is so sensitive due to the haemophilia. Nowadays, such severe joint damage should no longer occur in haemophilia. And we can be confident that they do not. However, these images from years gone by are a reminder to look after these patients well and to understand the challenges of therapy. Haemophiliacs have been brought to the attention of the general public by a sad fact: when too little was understood about AIDS, these patients were infected with the coagulation disorder through blood products obtained from HIV carriers.
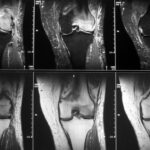
11 / Tibial shaft, stress fracture, MR

| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
11. 28-year-old decathlete, after an enforced break from training and a longer period of intensive training. T2 gradient echo and T1.
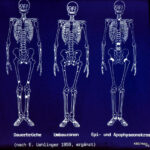
12 / Similar regions for fatigue fractures, remodelling zones and epi-apophyseal necrosis. Scheme modified according to E. Uehlinger, (born in Schaffhausen, worked in Zurich, temporarily in St. Gallen)
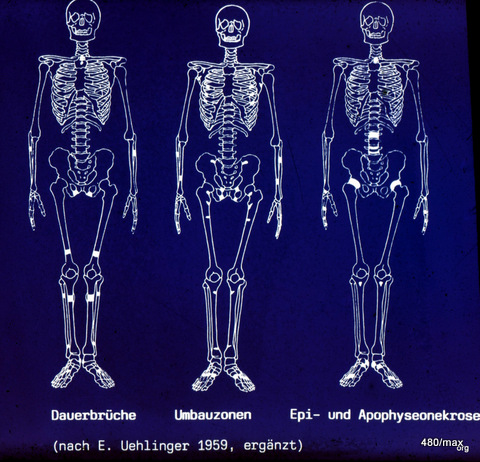
Uehlinger made this drawing a good 50 years ago. In it he compares
- Permanent fractures (chronic trauma on healthy bone),
- remodelling zones (chronic trauma on diseased bone),
- Epi- and apophyseal necrosis (chronic trauma (?) to particularly sensitive juvenile bones).
All are in similar regions: those that are particularly stressed and at risk, e.g. due to the upright gait.
However, there are differences in the respective point of attack, which varies depending on the age of growth:
In the case of epiphyseal and apophyseal necrosis, it is the growth plates, neighbouring metaphysis and bone cores.
In the case of permanent fractures and remodelling zones in adults, it is the shaft area of the bones.
In the regions where one of these entities occurs, other entities can also be expected at a different age or with a different state of health of the bone.
Example: The “Schipper fracture” (a permanent fracture of the spinous process at the junction of the cervical spine and thoracic spine) was well known. This overload fracture in adult healthy men mainly affected the shaft of the spinous process (preferably at D1 = 1st thoracic spine).
H.G. Schmitt (1907 – 2000) proved that there is also a disease at a certain growth age that affects the tip of the spinous process (again preferentially at D1 = 1st thoracic spine). He carried out very careful observations and showed that at this age (12-14 years) it is not the shaft that reacts but the growth nucleus, the growth plate and the apophysis close to the growth plate. There are characteristic healing patterns of this disease. This observation was confirmed in various parts of the world and named H.G. Schmitt’s disease. It could be interpreted in different ways.
<blockquote
- According to the X-ray image, this was an inflammation = apophysitis, the bone was irregularly destroyed, dissolved and reacting with healing processes.
- According to the pathological anatomy, this was apophyseal necrosis.
- According to the anamnesis – all had undergone unusual and excessive work and sports activities – it was overload damage to the juvenile spinous process. (H.G.Schmitt)
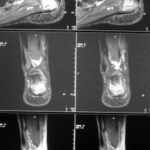
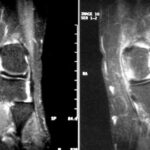
13 a / Fracture of the distal tibia (shin bone), fibula (calf bone) only compressed. MR here with T1 sequences
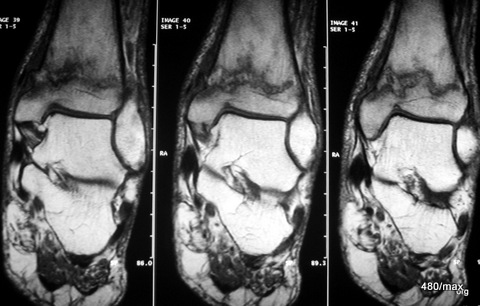
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
13th adult male with a car accident (totalled). I cannot quite reconstruct why this MR examination was performed. The X-ray examination clearly showed a fracture in the distal tibia without any significant displacement of the fragments. Perhaps the aim was to obtain more detailed information about the capsular ligament apparatus in the ankle joints or the involvement of other bones (e.g. talus).
13 a: MR: T1 in coronal slice guidance. In the fracture zone, the fatty tissue is displaced, the contour of the tibia is raised on the medial side. The tibia and talus as well as the large ligaments – insofar as they are included here – are inconspicuous. The fine dark lines in the calcaneus correspond to bone beads.
The following images (b – d) show T1, gradient echo T2 and STIR again. Memorise the character of the images well.
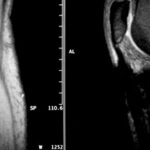
13 b / Same case. MR: also T1
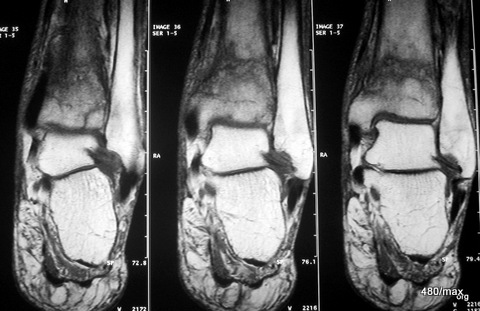
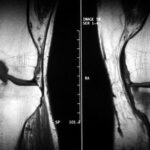
13 c / MR: Gradient echo; in sagittal stratigraphy.
13c MR of the same patient as a gradient echo; in sagittal slice guidance. Typical for this gradient echo is a T2 weighting with extensive (here not complete) suppression of the fatty tissue and good detail resolution. The fracture is clearly recognisable, the anterior and posterior compacta of the tibia is bulging; the haemorrhage and swelling of the soft tissue is only moderate; slight effusion in the upper and posterior compartments of the lower ankle joints.
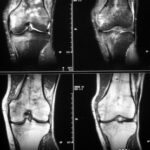
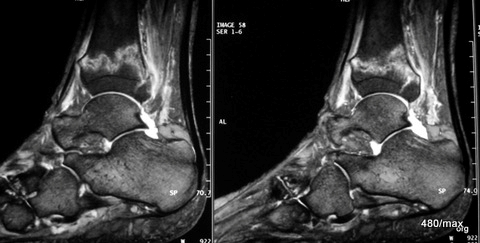
13 d / Still the same patient with the fracture of the distal tibia. MR: STIR in sagittal slice guidance.
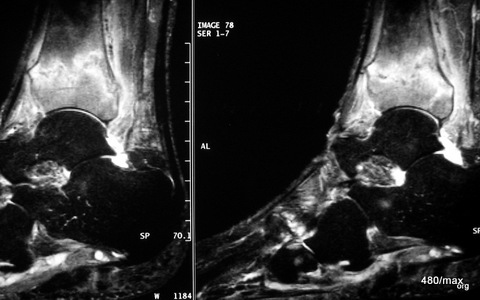
13d. MR: STIR in sagittal slice guidance.
The full extent of the noxious agent in the bone and soft tissue can be seen here through the sensitively visualised increase in fluid in the bone and soft tissue. Although the detail resolution here is less good than in the gradient echo sequence, the contrast between the strongly suppressed signal of the healthy bone and the pathologically bright signal in the fractured bone (and the surrounding soft tissue) is particularly clear. This sequence is well suited to not overlook small traumas. Sometimes SRIR is thought to be exaggerated, it could mask the main findings. This is one reason why very experienced diagnosticians in particular warn not to overestimate STIR.
A slight oedema can also be seen in the distal fibula, an additional fracture of the fibula could not be proven in the course of the procedure. Further images provided information about the ligaments including the syndesmosis between the distal tibia and fibula, this syndesmosis was not ruptured.
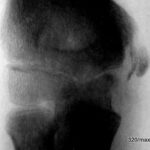
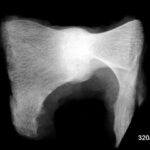
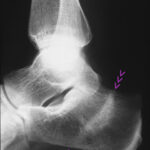
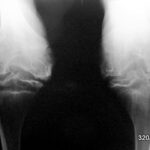
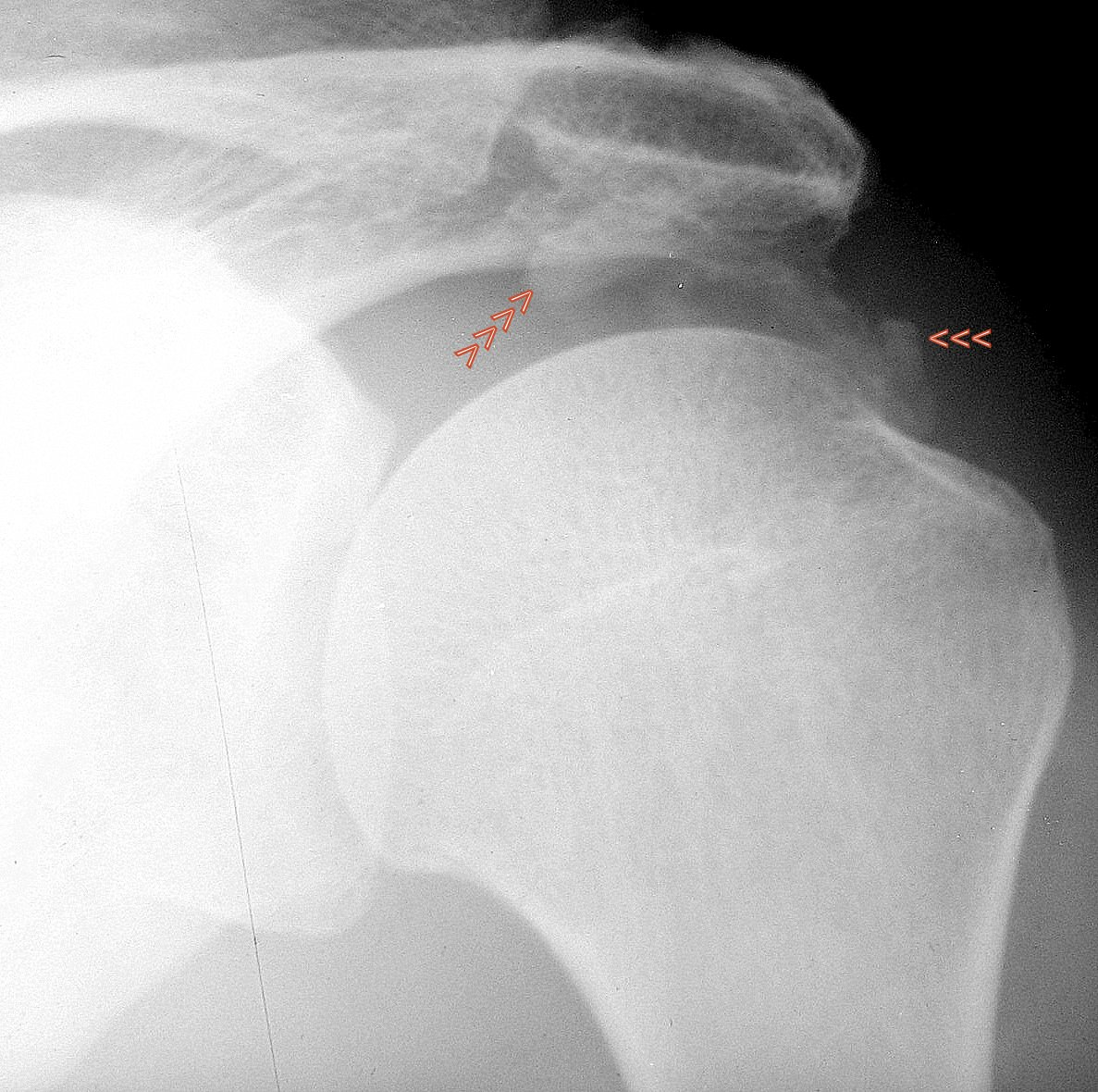
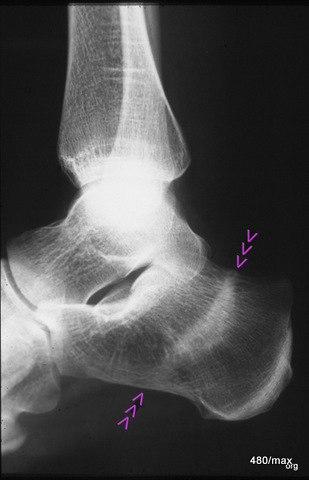
14th stress fracture of the calcaneus. Here in the X-ray, lateral beam path
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
14. 40-year-old patient jogged for an unusually long time in new trainers and with new good intentions. Several days later he felt unusual pain in his heel bone, which made it impossible for him to step firmly. Another X-ray examination was carried out several days later. At this point there was very valuable information, namely that the pain had already improved significantly.
X-ray examinations often don’t make things as easy for us as MR, especially STIR (as above). You have to look for a suitable case that you can demonstrate nicely, like this one, and leave the critics no chance (“play of nature”, “incidental finding”…). The bone must have already reacted clearly; and this juxtaposition of degradation and regeneration,
In this lateral X-ray image, the irregular compaction zone in the centre of the calcaneus is marked by arrowheads. The normal bony beams appear thickened and blurred.
This X-ray image, combined with the stress history, further combined with increasing improvement, is evidence of a stress fracture. Anyone who still does not believe it will be convinced by the disappearance of the change after a longer period of time. In a few months, it is very likely that the compaction zone will have disappeared and the calcaneus will be completely normal.
In this case, the “healing component” outweighed the destruction of the bone.
Such a course was demonstrated in the article on radiation protection. However, this was not a healthy bone, but a support system that was probably weakened and vulnerable due to many years of polyarthritis.
15 / Further stress fracture of the calcaneus
(German: Kalkaneus), more difficult to recognise.
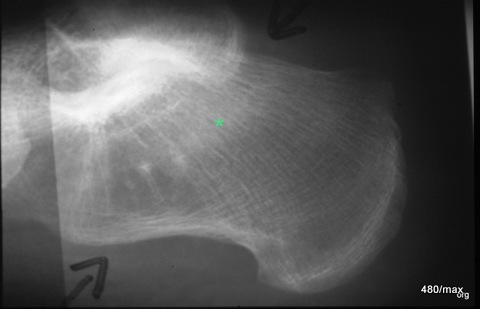
15. 56-year-old woman with a typical history of overuse and typical pain findings.
Lateral X-ray of the calcaneus. Apart from minor degenerative changes in the lower ankle joint, a blurred compression zone marked with a green star. This finding is difficult to recognise. Only the clinical course with increasing improvement with rest and the disappearance of this finding at a check-up after four months proved that this diagnosis was correct.
Should an MR have been performed? Then the findings would have been obvious (or would they have been ruled out?). The necessity of an MR is a question of temperament, experience and available resources; it does not seem absolutely necessary to me in this case. I am convinced of the diagnosis.
16 / Stress fracture calcaneus, MR in different sequences

| Akutes Trauma | im Wachstum | gesunder Bandapparat? |
| Chronisches Trauma | Ausgewachsen | Vorschaden ? |
16th adult woman with no previous skeletal system disease. Classic history of overuse and no evidence of acute trauma.
MR only in the centre, STIR with the typical suppressed fat signal in the healthy bone. The pathology shines brightly: large oedema zone in the central and upper calcaneus, which is crossed by a dark fracture line. – It is often not possible to explain in detail what exactly causes the dark signal in the fracture area. Apparently it is blood components and the regenerating new bone formation.
Remaining images T1 in different layers. Here the healthy bone is light-coloured, unless the pathological process has displaced the fatty marrow.
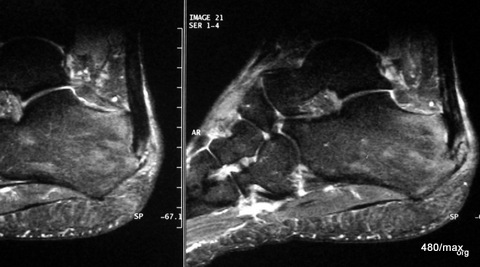
17 / Tendinitis in the insertion of the Achilles tendon and bone marrow oedema, MR: STIR.
| Akutes Trauma | im Wachstum | gesunder Bandapparat? |
| Chronisches Trauma | Ausgewachsen | Vorschaden ? |
17. 39-year-old man. A particular strain in his medical history is not readily recognisable. There is a pelvic obliquity, moderately pronounced tilt-splayfoot, diabetes mellitus, overweight approx. 15 kg. Initially minor, then more severe pain in the heel and in the area of the Achilles tendon.
MR as gradient echo sequence, sagittal slice guidance.
Noteworthy is the fluid retention in and around the distal Achilles tendon, also in the soft tissue, and slight patchy oedema in the calcaneus. Diagnosis of tendinitis of the Achilles tendon in the insertion area and overload reaction in the calcaneus.
What is instructive about this case is the fact that “Achillitis” is not limited to the tendon, but also includes the surrounding functionally involved structures.
Stretching exercises were carried out, the difference in leg length compensated, insoles prescribed, inflammation radiotherapy with 5 x 1.5 Gy. Continued quite successful weight reduction by avoiding various hidden and obvious sugars in the diet. Reduction of excessive breakfast.
Hesitant, but nevertheless continuous and ultimately clear improvement in findings.
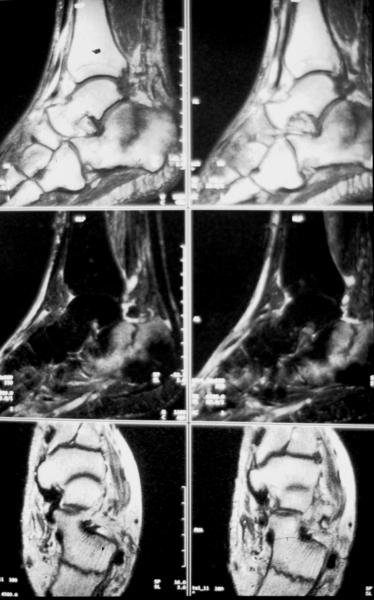
18 / Fracture of the calcaneus, MR
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
18. no previous damage, 39-year-old man, fall from the basement stairs.
MR: top and centre T2 weightings, bottom T1.
By now, dear reader, you already have a good eye for the different MR images of the bone marrow: light in the T2 weighting, dark in the T1 weighting, the fracture line is dark in both sequences. A coarse shell-like fragment has been knocked out on the medioplantar side of the tuberosity and is only slightly displaced. The patient was treated conservatively.
The injury has healed well functionally and morphologically.
The parameters are different, but we are still in the field of osseous insufficiency and will remain so for almost all of the next 40 cases.
II Pelvis, hip joint, thigh 19 – 39
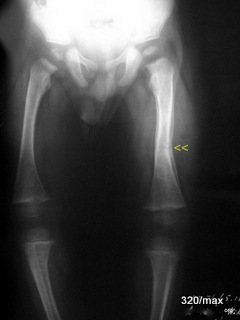
19 a / (+b). Rhachitis thigh left chronic fracture
| Akutes Trauma | im Wachstum | gesunder Kn.+ Sehne |
| Chronisches Trauma | Ausgewachsen | sekundär.kr.Knochen |
19 What a drastic change from the last case of the disease. Rickets is typical of childhood. The counterpart in adulthood is osteomalacia. In both cases, the osteoid (the non-calcified bone substance) does not “want” to “form bone” properly. It accumulates, pushes up the bone and lifts the periosteum (the bone skin).
This case of illness occurred a long time ago. This poor child is suffering from a severe vitamin D deficiency.
You should note these X-ray symptoms: cup-shaped metaphyses, bending of the bone shafts up to fractures (“green wood”), remission lines. Pay attention to 18. A, the damage in the bone cores can only be guessed at in this image, the calcification of the growth plates is disturbed, impressive periosteal reactionin the left femur and insidious fracture. Gradual fracture slightly distal to the centre of the shaft: slight axial misalignment with an outwardly open obtuse angle (arrowhead).
Such severe bone damage caused by vitamin D deficiency is now a thing of the past. Nevertheless, we need to know about them, also in order to understand such clinical pictures in regions of the world where there is great need.
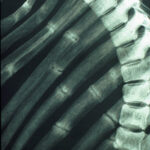
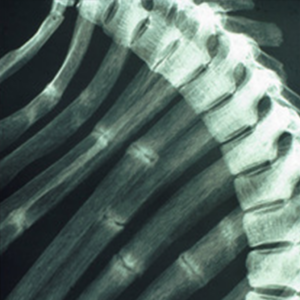
In Fig. 19. b, the same small patient: periosteal reaction of the rib in rickets. This additional line cannot be explained by the physiological sulcus of the rib (as will be shown in a separate article on the normavariants of the thorax). Not so obvious is the rachitic rosary: the bulbous distension of the ribs near the bone/cartilage junction.
Note: The differential diagnosis of periosteal reactions on X-ray also includes rickets.
The unfortunate child would have benefited if it had been born later, when more was understood.
19 b. the same sick child; rickets, periosteal reaction of the ribs
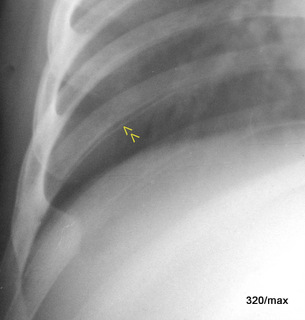
20 a / No vitamin D deficiency; Perthes’ disease; b – d: course of 1 ¼ years.
| Akutes Trauma | im Wachstum | gesunder Kn.+ Sehne |
| Chronisches Trauma | Ausgewachsen | sekundär.kr.Knochen |
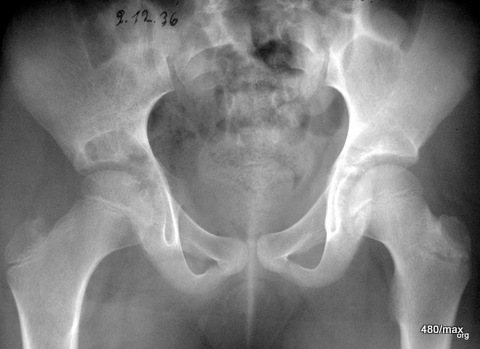
20 b / Perthes progression, collapse of the femoral head; all X-rays
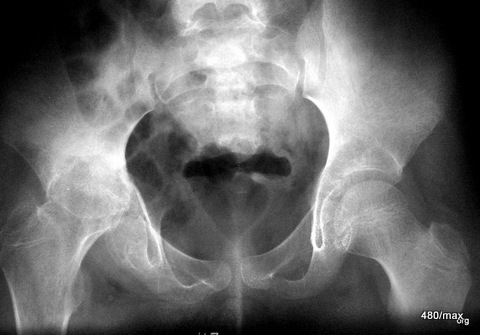
20 c / Perthes progression, X-ray As the disease progresses, the joint is increasingly destroyed and the head shortens.
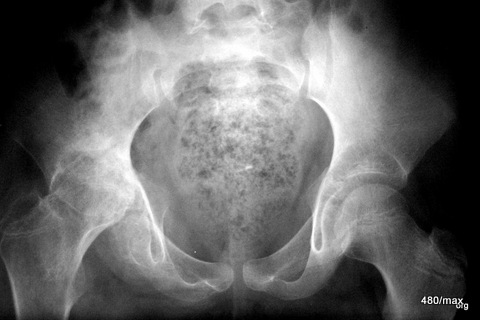
20 d / “Perthes”; X-ray course already after 1 1/4 years severe destruction of the joint, deformation of the femoral head and the growth plate.
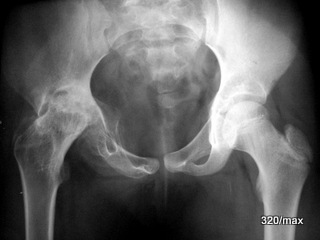
20th historical case of a 9-year-old girl (the archives had to be searched; the pictures are valuable and it is important for our understanding not to forget the “X-ray “); the special thing about this girl is the X-ray course, 12/1936; 6/37, 8/37, 2/38.
No vitamin D metabolic disorder, no other generalised bone disease. There is no acute trauma. Nevertheless, increasing hip pain and limping on the right.
Initially, only some decalcification in the epiphysis was noticeable. In the further course of the disease, the femoral head collapsed, and in the acetabular region there was marked structural coarsening and pronounced sclerosis. The joint is increasingly destroyed, the head is shortened, the socket is rounded and considerably deepened.
General information about Perthes’ disease (Georg Clemens Perthes, surgeon, 1869 – 1927, from 1910 in Tübingen), affects children between the ages of 4 and 8, boys more than girls.
The location is the epiphysis, growth plate and the metaphysis close to the growth plate.
Bilateral involvement in one third of cases (if simultaneous and delayed involvement are added together: synchronous + metachronous).
Bilateralinvolvement is therefore not quite as common as in femoral head necrosis (HCN).
Staging of Perthes (similar to HKN):
- Initial stage without X-ray findings.
- Stage of “whitening” * and sclerosis, i.e. necrosis and repair.
- Stage of defect healing with coxa vara and arthrosis.
* (The radiological nomenclature is somewhat difficult, see “Radiation protection”.
MR is predominantly welcomed as important information (I am not showing a patient for reasons of space). When using MR, you have to find the right balance here too (Riggs).
In any case, the originally high T1 signal of the epiphysis is reduced. The T2 signal is rather low due to a connective tissue component in the case of disease, the hyaline articular cartilage is rather thickened, the membrane of the synovia is widened.
21 / Age distribution: vitamin D deficiency and starvation osteomalacia.
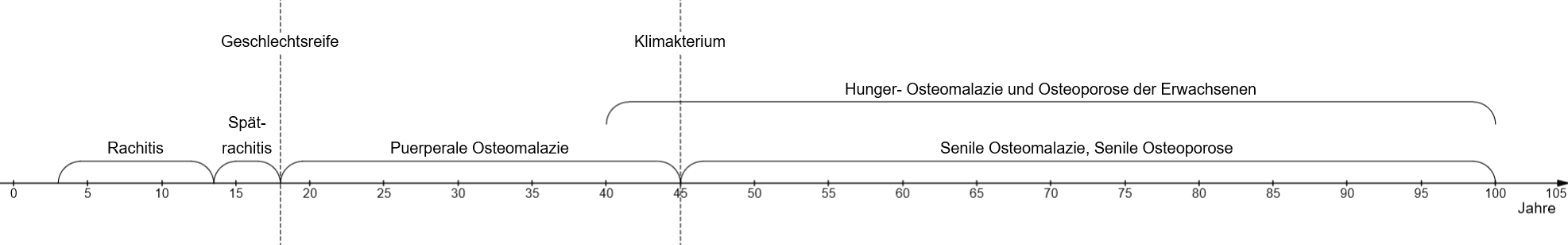
This is how H. G. Schmitt (1907 – 2000) saw the age distribution of vitamin D deficiency diseases (rickets/osteomalacia) and starvation-osteomalacia 80 years ago.
In the post-war period, but also during World War II, there was endemic vitamin D deficiency and there was a high incidence of vitamin D starvation. World War II, there was endemic vitamin D deficiency and malnutrition.
It was life-threatening to talk about this under the Nazi regime. After the fall of the dictatorship, the Allied occupiers also did not like to hear that there were difficulties in feeding everyone well.
We should not forget these diseases (rickets/osteomalacia), which have become so pleasingly rare in Europe today. There are still emergency areas in the world. Advice to all those who help out in regions where people are fleeing and starving: a first indication is pressure pain over the sternum and tibia).
There are probably strong links between the two clinical pictures. What they have in common is insufficient mineralisation. People suffer from persistent pain, sensitive periosteum, loss of strength and a feeling of illness.
The X-ray findings are non-specific for a long time and only show decalcification as in osteoporosis. Only the remodelling zones, the creeping fractures so to speak, are spectacular. MR can also detect these and even very early.
There is also a predisposition to acute fractures in osteomalacia .
In addition, chronic diseases occur more frequently.
The difficulty is that osteomalacia can be mixed with osteoporosis in the elderly.
Even today – and even in industrialised countries – vitamin D deficiency is not uncommon in the elderly. What will the situation be like in regions with nutritional deficiencies?
Vitamin D deficiency can be detected in the laboratory.
Treatment with vitamin D and calcium has few contraindications.
Daily vitamin D doses, which are given in IU, are preventive. They are below 1000 IU, even if they increase with age. Some say 1000 IU (one vigantolette) is not wrong, especially if someone gets too little sun.
Hypophosphatasia, defects in “alkaline phosphatase”, should be distinguished from classic osteomalacia. If the enzyme does not function, pyrophosphatase prevents bone mineralisation. This is a dangerous childhood disease that can jeopardise breathing due to the soft rib thorax. Partial dysfunction also occurs in adults and is associated with bone pain and stress fractures. Arthritis and chondrocalcinosis occur.
It can probably be said that malnutrition, as it occurred and still occurs in times of hardship, posed a particular risk for osteomalacia in the elderly. It is likely that the two conditions overlap or are even identical. Today, these bone diseases caused by hunger should be a thing of the past. It is important to realise that such diseases are to be expected in emergency areas. It is also important that there was starvation osteomalacia in our country.
22 / Child, condition after hip dislocation on the right, condition after repositioning (reduction)
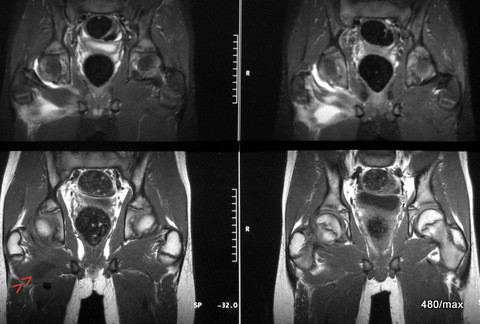
| Akutes Trauma | im Wachstum | gesund. Kn. Weicht? |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
22 The boy suffered a dislocation of the hip joint in a car accident. Overall a rare dislocation. This was repositioned skilfully.
As far as I know, the function was good, no motor or sensory deficit.
It is not surprising if you are not in top form the next day after a hip dislocation. It was too slow for those involved and they arranged for an MRI. No surprising findings. We have the opportunity to see that the soft tissue is involved in such an injury. Please describe the localisation of different types of haemorrhage.
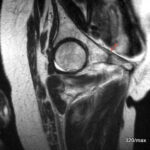
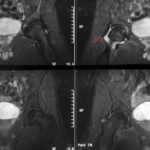
23 / New case of illness. Overload with hip joint effusion. MR top STIR, bottom T1 KM (gadolinium): In this sequence, only perfused tissue is imaged brightly.
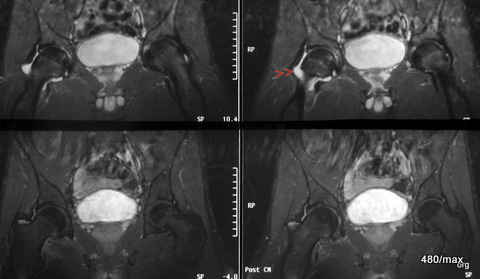
| Akutes Trauma | im Wachstum | gesunder Knochen? |
| Chronisches Trauma | ausgewachsen | kranker |
23. 24-year-old athlete, very intensive endurance training on hard surfaces, sometimes with inclines. Beginning degenerative changes in the hip joints. Subsequent loss of sensation in the right hip, feeling of numbness and unsteady gait.
Two interesting (only apparently similar) sequences: T1 fat-saturated after intravenous contrast agent
In the STIR, the urinary bladder is intensely bright, and there is also a clear joint effusion around the femoral neck (arrowheads).
The two images below show a completely different sequence. Here the urinary bladder contents are also bright (should be dark at T1), but irregularly bright; this is contrast urine flowing into the urinary bladder. KM causes – where it reaches – a bright signal. The hip joint effusion is not supplied with blood and is therefore not depicted brightly. Only the peripheral areas of the capsule show increased blood flow.
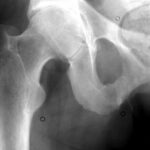
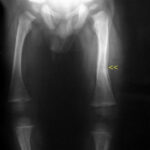
24th new case of the disease. Aseptic femoral head necrosis (HCN or ischaemic HCN) on both sides.
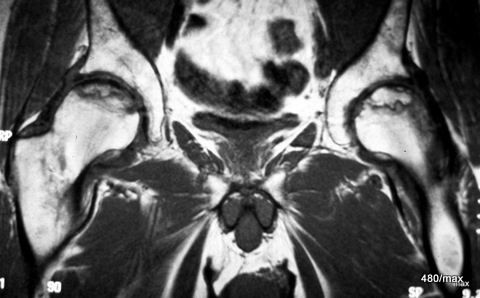
By now you, dear readers, are so well versed that you can make the classification in the six-step scheme: Mature bone, chronic trauma and a strange vulnerability of the bone.
24. 54-year-old patient, 3 years of cortisone medication due to bronchial asthma, slowly progressive pain in both hip joints.
MR T1 (contrast agent was not administered, see the dark bladder contents): typical limitation to the heads of the femurs, namely to the pressure absorption zone; the predilection site of the HCN is the cranial/anterior/medial segment.
Typical is the recess of the acetabulum and in particular the acetabular roofs (unlike in activated osteoarthritis).
Apparently a coexistence of necrotic and regeneratively active zones. Typical map-shaped zones. In further sequences, these are shown to be partially supplied with blood and partially excluded from the blood supply.
This large chapter on hip joint necrosis should be illustrated with numerous images. Here we have limited ourselves to the very first impression. In any case, MR is excellently suited for this entity.
General comments on HCN:
In contrast to “Perthes”, aseptic femoral head necrosis is a disease of adulthood, 3rd to 5th decade of life (four males per one female).
Symmetrical involvement in 70 % (simultaneous + delayed) is more frequent than in Perthes and more frequent than in fatigue fractures.
The causes are so varied that it must be assumed that we do not have a conclusive picture of this aetiology. Acute or chronic trauma plays a special role. However, there is also an accumulation of HKN in:
⦁ Cortisone medication,
⦁ Collagenoses,
⦁ Caisson’s disease,
⦁ Pancreatitis,
⦁ Hyperlipidaemia,
⦁ Sickle cell anaemia,
⦁ Diabetes mellitus,
⦁ Alcohol abuse,
⦁ Gaucher’s disease,
⦁ Hyperuricaemia,
⦁ Polycythaemia vera,
⦁ Haemochromatosis,
⦁ Lupus erythematosus,
⦁ Or nothing of the kind is found = idiopathic form.
This list shows that there are many risk factors for cardiovascular diseases. However, these diseases occur around 20 years later. In addition, there is an accumulation of conditions that also favour fatigue fractures (chronic fractures).
Caution: In the discussion, “bone marrow” is used synonymously for completely different tissues:
Haematopoietic cells (necrotic after 6 to 12 hours)
Cancellous bone cells (necrotic after 12 to 48 hours, not detectable in MR, Nagel’s experiment)
Fat cells (necrotic after 3 to 5 days)
The most common classification is that of Ficat, which was developed before the MR era:
0 = histological evidence only
1 = clinical findings only in the absence of X-ray findings
2 = clinical + X-ray findings added (with combination = lysis + necrosis)
3 = stronger clinical and pronounced X-ray findings: subchondral fracture (increasing = crescent sign)
4 = “deformity/arthritis”
MR as early as Ficate stage 1 opened up the possibility of earlier diagnosis and thus the hope of avoiding necrotic collapse of the calotte (…. up to irreversible stage 4).
The advantages of MR and scintigraphy over X-ray are undisputed. A lot of literature on the subject of MR or scintigraphy: MR has (only slightly) higher sensitivity (is there something pathological?), but significantly better specificity (what else could it be?).
CT only plays a part in this orchestra in this respect: It is superior to X-ray in the detection of subchondral fractures, inferior to MR in soft tissue diagnostics.
Fatty tissue dominates the MR signal, it is impressively high in both T1 and T2, as SE! If the healthy fat is displaced by oedema (in the broadest sense), this results in an abnormality in the T1, but also in the fat-saturated T2, e.g. in the STIR.
It is essential to distinguish between the central section of necrosis and the marginal area. According to Mitchell, this central section of necrosis is composed very differently. The following signals in different images, but also a “colourful” mixture:
1. Fat: T1 high, T2 moderately high
2. Subacute haemorrhage: T1 high, T2 high
3. Fluid: T1 low, T2 high
4. Fibrosis: T1 low, T2 low
However, the extent of the necrotic process rather than the centre is important for the prognosis of the necrosis. It is favourable for surgical treatment if the necrosis is not too large. With KM-enhanced MRI, we expect no enhancement in the centre of the necrosis and significant enhancement in the peripheral area.
The boundary line of the necrosis to the healthy bone is striking in the T2 image = the double-line sign is detectable in the majority of cases:
signal-rich line on the side of the necrosis and
low signal towards the healthy marrow.
The latter is probably the hypervascularised repair zone and the fibrosed/sclerosed zone.
Indications for MR in suspected HCN are
⦁ Absence of X-ray findings with persistent clinical symptoms
⦁ Differential diagnosis in the absence of X-ray findings
⦁ Extension and collateral involvement in the presence of confirmed findings
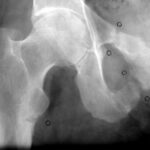
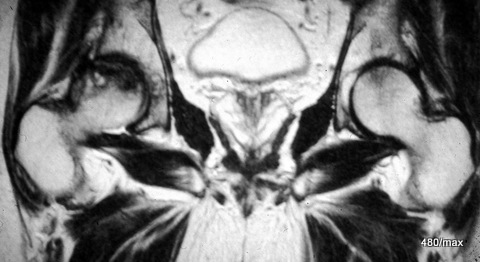
25 / Another case of necrosis of the femoral head on the right, in MR T1 without fat saturation after administration of contrast medium.
| Akutes Trauma | im Wachstum | gesunder Knochen? |
| Chronisches Trauma | ausgewachsen | kranker |
25 As I said, necrosis of the femoral head is a large chapter in its own right. The intention here is only to touch on this topic with a few MR images.
It is also clear here in a 43-year-old man that the joint sockets are spared from the pathological process, the right firing head is excluded from the blood supply in the characteristic pressure recording zone. The contrast medium is very bright in T1. Blood flow or lack of blood flow is very clear. There are individual perfused spaces that clearly accumulate the contrast medium. This becomes even clearer in a fat-saturated T1 sequence.
Here, bone damage is shown which, in contrast to Perthes, affects the adult femoral head. As with Perthes, the bone has a predisposing weakness of some kind.
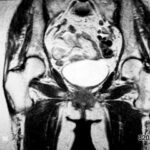
26 / Transient osteoporosis. A mysterious clinical picture; MR has helped to publicise it.

| Akutes Trauma | im Wachstum | gesunder Knochen? |
| Chronisches Trauma | ausgewachsen | kranker |
26. 49-year-old man (age and sex atypical here), unusual work, overall no typical history, pain in the hip joint.
MR: The image shows STIR at the top and T1 at the bottom. We see an extensive, very characteristically arranged oedema in the entire femoral head, in the femoral neck and in larger sections of the trochantermassif. This oedema is characteristically light in STIR and dark in T1. Here too – as with femoral head necrosis – the acetabulum is uninvolved. The capsule and the neighbouring soft tissue react only slightly.
What you need to know summarised: Transient osteoporosis (TO) is a rare clinical picture. The reduction of calcium salts in the head and neck of the femur is not easy to objectify with conventional X-rays, but with the use of MR we have striking, eye-catching findings:
Medullary oedema is best shown in STIR, in decreasing clarity in GSE, TSE up to T2 in SE. An important addition is “fat-saturated T1 after administration of KM” (differentiation from all forms of coxitis).
TO was initially thought to be a disease of young women. (age distribution between Perthes and HKN). More recently, it has also been observed in men of older age. See our case.
As a rule, TO is apparently an independent clinical picture that is benign and regresses in 6 to 12 months.
The aetiological discussion is not closed. Is TO only a preliminary and intermediate stage of HKN? Vahlensieck observed TO on one side of the body and HCN on the other.
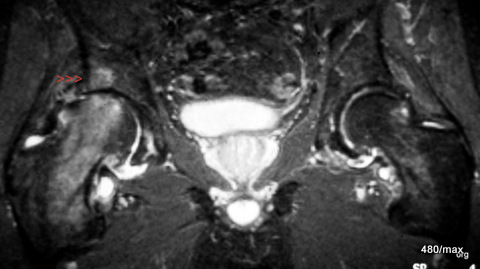
27 / Activated osteoarthritis of the hip joint
| Akutes Trauma | im Wachstum | gesunder Bandapparat? |
| Chronisches Trauma | Ausgewachsen | kranker Knochen + Gelenke ? |
27. 68-year-old patient with right-sided coxarthrosis known for years. Much more severe pain for 5 weeks. The underlying cause is dysplasia of the joint socket: the pressure absorption zone is too small and predisposes to joint damage.
MR: This STIR image is not pretty, but it shows the extent of the pathology without special tricks and clarifies the differential diagnosis.
We can see the coarse marginal ridges on the head and acetabulum and the higher degree of joint space narrowing, more on the right than on the left. The joint effusion is also more pronounced on the right. On the right side, there is pronounced oedema in the head of the femur (proximal femur), emphasised in the pressure absorption zone. The key point for the diagnosis is the fact that there is also a small oedema in the acetabulum (red arrowheads). The latter would be atypical for transient osteoporosis, as would the age and history. This is an activated osteoarthritis of the hip joint.
General observation:
Osteoarthritis has been neglected in my report so far. Isn’t osteoarthritis also the product of an imbalance between stress and resilience? These correlations aren’t rock solid. You would have to be able to prove this for any osteoarthritis: On the one hand, there was an unusual strain combined with a susceptibility of some kind. Thus, the focus is limited to the latter and the stress aspect is neglected.
There are undoubtedly risk factors for osteoarthritis:
⦁ Age
⦁ Obesity
⦁ Joint diseases such as gout, psoriasis, chronic polyarthritis
⦁ Particular occupational stresses such as ballet, parquet laying
⦁ Stresses in daily life such as unhealthy (fashionable) shoes
You should delve deeper into this topic. I have only done it with one case. In this case, the osteoarthritis was present and the bones/joint were additionally damaged by overloading. In other words, the stress reaction to osteoarthritis: activated osteoarthritis.
28 a / New: Chronic left femoral neck fracture. MR: Which sequence is shown?

| Akutes Trauma | im Wachstum | gesunder Knochen? |
| Chronisches Trauma | ausgewachsen | kranker |
The 68-year-old doctor has been hiking in Liguria. It’s difficult terrain with inclines and rocky descents and long detours due to landslides.
It’s so beautiful that she wanted to make the most of her time. At some point towards the end of her stay, it was too much. Severe pain set in. There was no anamnestic evidence of an acute injury. Consequently, we were not surprised:
No step, no shortening in the femoral neck, no whitening line to be seen! The pathological findings were difficult to see on the x-ray! The presence of a special form of fracture was not believed. Here, in the MR, it is proven, so to speak (some say“foolproof“).
By now, dear readers, you are so practised that you can recognise the following MR sequence of the same patient:
Fatty tissue light, bladder contents dark. A broad “oedema” in the centre of the femoral neck draws a black line through the femoral neck = T1:
28 b / The same patient. The chronic femoral neck fracture is shown with which sequence this time?
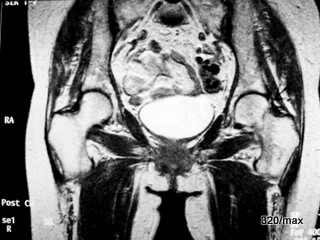
T1 again? That could fit if the bladder contents were not suddenly very light in colour. It is T1 after intravenous contrast medium: The zone of bone marrow oedema or is it better described as a reaction zone is brighter; what makes it brighter? Expression of an injury and healing process? What has gained brightness? Here, a regenerative process is underway with blood flow.
Of course, this could also have been shown “fat-saturated”, which would have emphasised the extent of the contrast agent enrichment even more clearly.
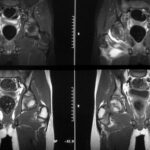
29 / Implantation of an artificial hip and subsequent signs of inflammation (especially CRP) and fever 39°C. Septic hip. MR: STIR = upper images and T1 after CM = lower images.
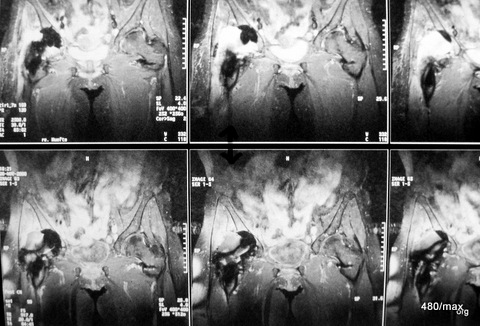
29 The special feature of the image are the two sequences that appear similar (?) at first glance. Only T1 after contrast (top) allows the
-non-vascularised (purulent) joint effusion to be differentiated from the
-vascularised inflammatory tissue
.
There is not yet enough contrast urine in the bladder to visualise it properly in bright colour.
Bottom STIR: It is difficult: The effusion (and the bladder contents) is bright in STIR and still partially dark in CM. Inflamed tissue is bright in both sequences.
This complication is rare. The lengthy medical history came to a – we hope permanent – conclusion with an explantation of the prosthesis, antibiotics for several weeks and finally a new implant.
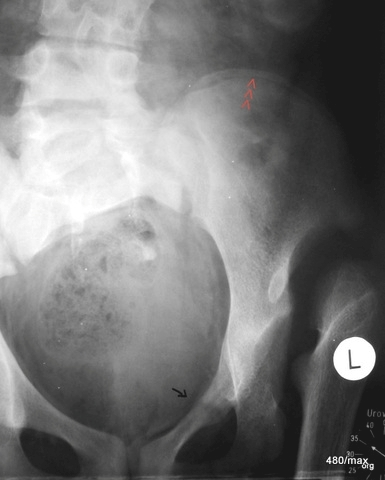
30 / 15-year-old girl; she suffered from renal insufficiency.
| Akutes Trauma | im Wachstum | gesunder Kn.+ Sehne |
| Chronisches Trauma | Ausgewachsen | sekundär.kr.Knochen |
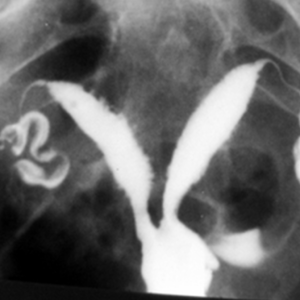
Congenital dislocation in the left hip joint, therefore incorrect loading of the pelvis. A Looser’s remodelling zone of the upper branch of the pubic bone has developed. (Looser is Swiss from Zurich, only the uninitiated pronounce it in English).
In this case there were two interacting causes of chronic trauma: the incorrect loading due to the deformed hip joints and the sensitive bone metabolism due to renal insufficiency.
The red arrowheads show a growth ridge in the iliac crest as a sign of skeletal growth that has not yet been completed.
Nevertheless, the remodelling zone is as developed as in adults. The case of the sick person tells us that the rules cannot be applied completely rigidly.
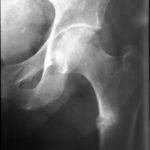
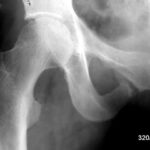
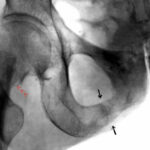
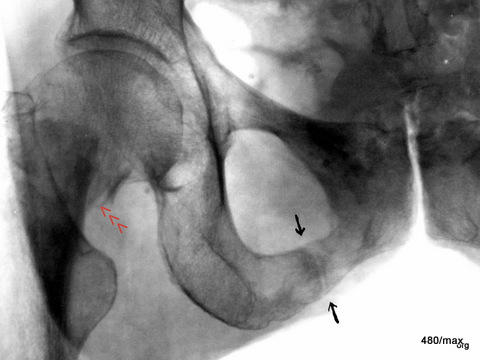
31 / Alcoholic. Remodelling zone in the lower branch of the pubic bone combined with an acute fracture in the femoral neck (the X-ray image is inverted: bone is dark!).
| Akutes Trauma | im Wachstum | gesunder Bandapparat? |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
31 The 42-year-old patient initiates a remarkable series with partly new, but also old observations; all are valuable:
He offers a highly interesting combination: a chronic and an acute fracture.
It is likely that such a linkage is rarely observed. But it must exist, and it is not at all surprising when such “related” diseases occur in the same region, but not at the same location (see E. Uehlinger).
The patient has probably already undergone multiple remodelling zones, e.g. in the upper right pubic ramus, near the central pelvic region. –
There is now aflorid remodelling zone in the lower branch of the pubic bone near the ischium (marked by black arrows).
The patient has fallen on the ice and sustained an acute fracture of the femoral neck. There is a considerable external rotation malposition of the distal fragment, which is why the crista intertrochanterica and the small trochanter are so clearly visible (see projection studies on the hip joint in “Radiation protection”).
These different traumas affect an alcoholic’s bone that has been damaged by vitamin and electrolyte disorders. Chronic and acute trauma occur in the same region, but on different bones.
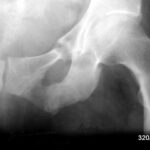
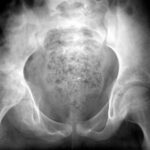
32 a/ Osteomalacia; we find Looser’s remodelling zones 4 times. The 4th is located in the lower branch of the pubic bone near the ischium (not marked in the picture).
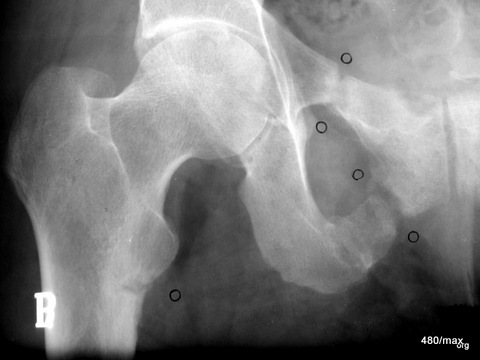
The following patients show particularly instructive Looser’s cases, which must also be known and recognised in the X-ray; first case 32 (a – c) in the course:
60-year-old nun, Sister Donatia.
She worked self-sacrificingly in a foundation in our town, was on a one-sided diet and there was no question of her getting the opportunity to go out in the sun. The onset of the clinical picture was dramatic with severe pain described as “in the abdomen and pelvis”, so that one could have thought of a metastatic bone process, or even ovarian cancer. The x-ray image shows Looser’s remodelling zones at least three times, probably even four times, i.e. very wide “fracture clefts” that are blurred by heavily sclerosed bone. This structure is completely atypical for acute fractures. The latter can also diverge, but the edges are sharp, pointed, without these neighbouring compressions (bright in the X-ray image).
Isn’t it fascinating that such chronic fractures can also occur as “piece fractures “? It can be assumed that all these phenomena that we are familiar with in acute fractures also occur in a similar form in chronic fractures. Chronic fractures are probably also observed in regions of the body where acute fractures are known and frequent. Sometimes we miss such observations; then we have to be very attentive to see if such observations are not made at some point.
This patient was diagnosed with a vitamin D deficiency, was given a high dose of D-vitamin and was relieved of her duties. In addition to the impressive medical history, there is an often unrecognised sociological history. Some clever people say that it wasn’t just the church that was guilty, the medical profession also looked the other way and was happy that someone was there to do the hard work, the “dirty work”. These are not just stories of the sick, but also stories of exploitation and lack of care.
The announced scheme is still missing:
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
32 b / “Looser” in the follow-up observation: improvement (clinical and radiological) did not occur immediately, but within a few weeks. After 6 months, the remodelling zones were already impressively built up and bridged.

32b. As a further special feature, we also discover a remodelling zone on the opposite side, on the left proximal femur.
As the remodelling zones in the femur are therefore found on both sides, some people talk about “Milkman syndrome”. Please avoid this term: by definition, overuse injuries can occur symmetrically. They even tend to do so. No need to name a syndrome. – This is the advantage of our far-sighted approach: the imbalance between stress and resilience comes in many different forms; it has many names. In the course of their working lives, the authors of these books have become so infatuated with the syndrome that they do not tolerate any broad comparisons being made. However, these comparisons help to achieve a greater understanding. Certain rules apply to all forms of osseous insufficiency! Thus the possibility of double-sidedness. Dear readers, please take my suggestion and avoid using the term “Milkman syndrome”. Even Milkman would be appalled by the misinterpretation of his observations and the misuse of his name.
32 c /Conversion zones, progress monitoring, healing.

32 c. After one year – only the right side of the pelvis is shown – the Looser’s remodelling zones were well healed and the bone was “built through”. –
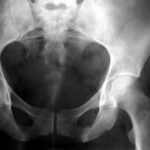
33 a (+b) / osteomalacia. This form is very rare nowadays.
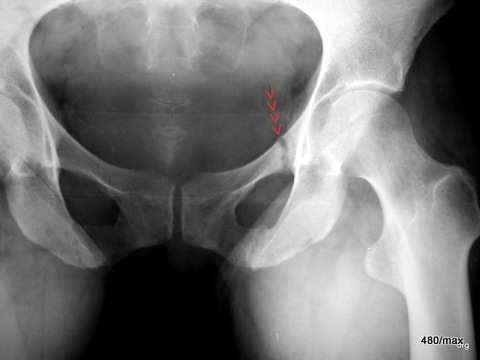
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
33 a and b. To make you believe that patient 32 was not an isolated case: another nun (only 40 years old). From the X-ray image, this case (Sister G.) could be confused with others. The eye has been trained in the meantime: The lower left branch of the pubic bone also has a remodelling zone; not so pronounced, perhaps beginning or already improved? Another Looser’s zone probably also runs through the right ischium.
This should also show that these are typical clinical pictures, the weak points in the bone are often similar with the same disease. So these diseases must and can be recognised, even if they have become rare in recent decades. We may see them again tomorrow or encounter them today in countries with famine or flight.
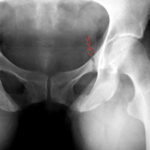
33 b / Progression of osteomalacia, same patient healed impressively after Vit D therapy and 4 months of patient care.

34 a / (+b) Looser conversion zones

| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
New case: 34 a + b. More of these interesting Looser’s remodelling zones. “Looser” can take on forms that make it uncertain whether osteolysis is present, as in a malignant disease. For patients and practitioners, everything turns out well in the end. The treatability of this 38-year-old woman was also very good. Picture after treatment (b) follows.
34 b / After treatment; the remodelling zones were also impressively bridged in this case of disease, one could also say that they were bony.
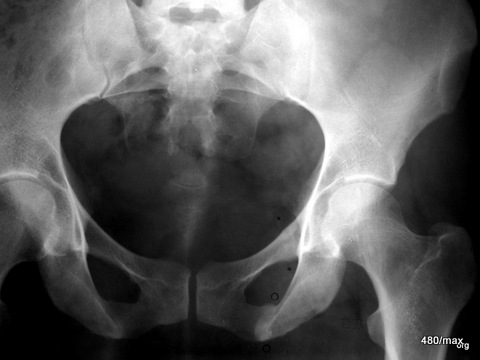
More of these interesting Looser’s remodelling zones. In the end, everything turns out well for patients and practitioners.
35 / fifth patient with osteomalacia
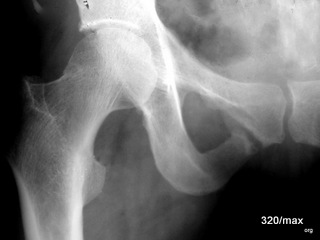
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
New case 35
A 36-year-old female patient with Looser’s remodelling zone (in the lower branch of the pubic bone, close to the symphysis). –
We have now spent more time on osteomalacia. There were cases from times of nutritional deficiencies, which now only occur very occasionally in Europe. Let’s not be lulled into a false sense of security that something like this will never happen again. Even if we are lucky enough not to experience epidemics, we will be confronted with such problems in problem regions of the globe.
For osteomalacia to really disappear, global politics must help. But the problem must also be known and recognised medically; this is where these patients help us, they train our understanding of the complex theory of disease. If you recognise their system, many things become simpler and easier to understand.
36 / Preparation of a Looser’s remodelling zone that has passed through

| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
During this patient’s lifetime, the cause of the change in the bone was puzzling. An accident was always denied. Several years ago, there was an episode of heavy labour despite low back and pelvic pain, which only subsided after a change in living conditions. A diagnosis was never made. The bone structure is regular and harmonious. A “fracture gap”, which is only hinted at, has been bridged over a wide area of bone and is heavily sclerosed.
An unexpected death occurred due to a pulmonary embolism. The histological examination confirmed: no evidence of a destructive process, such as a bone metastasis or a primary tumour, such as an osteosarcoma.
37 a + b / A completely different history: rear-end collision with acute fracture of the upper branch of the pubic bone.
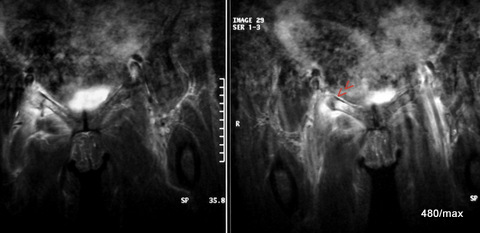
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
The images of this case are not as interesting and unusual as the previous cases. Bone fractures are common and it is unusual to diagnose them with MR. The examination was probably also unnecessary. The medical history is more important than these MR images.
(In other cases of illness (e.g. necrosis of the femoral head, transient osteoporosis) we did not want to do without MR).
38 / A completely different story with an accident in the swimming pool.

What should the scheme look like?
Acute trauma during growth Healthy bone
38. now to an acute trauma
A healthy adolescent jumped from a 10 metre board and hit the surface of the water with his thigh: the abrupt stretching of the thigh not only caused brutal shock and pain, but also an injury, an avulsion of the small trochanter (rolling hill) on the femur. An excessive counter-movement (stretching) of the thigh has torn out the bony attachment of a large tendon. The associated muscle lifts the thigh and flexes in the hip joint. (Laypeople call this the “loin”.)
In such cases, a decision must be made as to whether the bony tear should be surgically fixed or whether to remain conservative. The body has an amazing ability to immobilise such a torn muscle, it often prevents severe displacement and allows healing with moderate deformity.
39 / Entropathy and alcoholism: remodelling zone in enteropathy
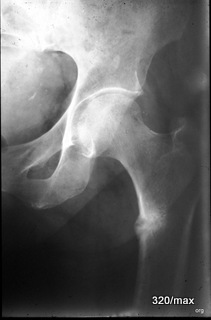
39 Back to a chronic trauma. This is what the scheme looks like now:
Chron. Trauma Adult diseased bone
We stay with the overview radiography = X-ray; 53-year-old man. Remodelling zone this time in the proximal thigh bone (femur; proximal means “near the centre”, in contrast to peripheral). Its bone metabolism is pathologically altered in alcohol abuse and enteropathy. The weakened bone reacts with a Looser’s remodelling zone to an everyday load that is too great for it.
Compare with case 31 and the following patients. All the “remodelling zones” could have been left together. They all have the same profile in the diagram: the three lowest boxes apply (= are marked in red). I wanted to show the diversity: all “osseous insufficiencies” can have different causes. They are similar and yet different.
III Differential diagnosis, discussion of growth plates, other cases of disease: Spine, ribs, sacroiliac joints,
knee, foot, shoulder, elbow, hand 40 – 63
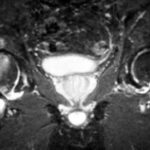
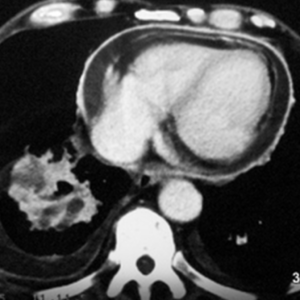
40 a / Bronchial carcinoma and metastasis in the right iliac bone (os ileum).
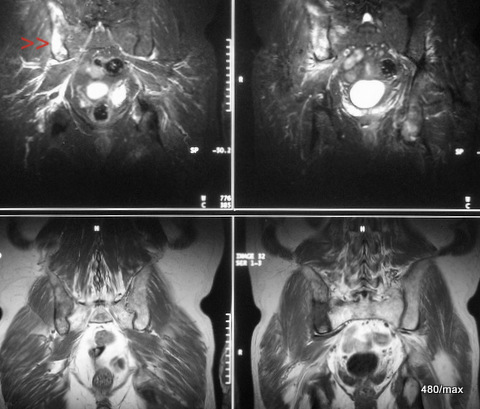
| Akutes Trauma | im Wachstum | gesund. Kn. Weicht? |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
40. a completely different disease in the bone.
Classification in our scheme of “osseous insufficiency” is not meaningful.
53-year-old patient. (There is good literature on the risk profile; elsewhere I have shown a chest x-ray of such a disease, the limited value of which for initial diagnosis has often been pointed out). The diagnostic possibilities are significantly improved by skeletal scintigraphy and magnetic resonance imaging (MRI):
Here MR: At the top of the STIR images, the sacrum and the left ilium extending upwards are completely dark. This is how it should be in this sequence and in the normal bone. The right ilium is strikingly bright, almost like fluid!
At the bottom of the T1, the contrasts are almost reversed: bone is bright like the “fatty tissue under the skin” and the centre of disease is rather dark.
Pay attention to the urinary bladder in STIR and T1.
The article “Bone metastases” describes how difficult it is to diagnose osteolysis on X-ray. It also shows a lysis in the sacrum, a case that keeps bothering me.
Some people will say: we wanted to talk about injuries in the broadest sense; a tumour disease doesn’t fit in at all! Correct.
Nevertheless, the (diffusely or circumscribed) metastatically affected bone is diseased bone. Its statics are reduced! Relatively minor trauma can break it (acute, but also chronic). This is referred to as a “pathological fracture”.
A buzzword? A fracture is actually always “pathological”. Where does a “pathological fracture” begin and where does it end? Are osteomalacic remodelling pathological? Fractures in Paget’s disease, in inflammatory pre-damaged bones/joints? The word “pathological fracture” should only be understood as an indication that the morphology of the fracture and the cause of the accident do not match. (“Insufficiency fractures” as
– chronic trauma with previous damage – are better defined).
41st daughter tumour prostate CA
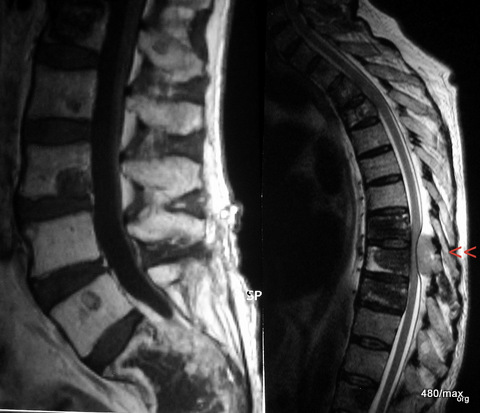
| Akutes Trauma | im Wachstum | gesund. Kn. Weicht? |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
Similar constellation.
Classification in our scheme of “osseous insufficiency” does not make sense.
41. The 70-year-old man with metastasised prostate cancer has metastases in all lumbar vertebrae and in the upper and middle thoracic spine. There in the thoracic spine (red arrowheads), an extradural metastasis compresses the dural sac from behind and presses on the spinal cord. What sequences are these?
Left: T1 without fat saturation but with contrast agent. The foreign tissue is significantly lower in signal than the normal bone. The KM slightly increased the signal of the foreign tissue. The difference to the normal bone was slightly reduced. If fat saturation had been used, the difference might have been masked. So: fat saturation is often, but not always, useful.
The image on the right cannot be a T1: The cerebrospinal fluid is bright! So a T2 weighting. Which one? According to the bright fat signal: SpinEcho-T2.
The foreign tissue in the vertebral bodies is irregularly structured and predominantly darker than normal bone, which is characterised by its marrow containing a lot of fatty tissue.
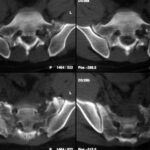
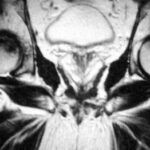
42 / Accident: fractures of the sacrum. Computer tomography (CT)
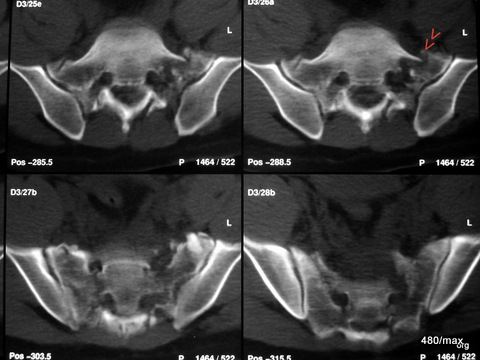
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
42. different history and use of a completely different method.
The 45-year-old used his tractor to uproot huge old trees. At one point, the tree was stronger and the tractor overturned backwards. A classic, extremely dangerous accident mechanism. The machine almost crushed the patient.
Here we see the computer tomography (CT) with extensive fractures in both massae laterales (the lateral parts) of the sacrum. The bone appears to be splintered, although 6 days have passed since the accident. There is still no recognisable reaction in the sense of incipient healing.
The diagnosis was difficult on X-ray (?) Or should stricter standards have been applied? After all, a contour interruption was found in one of the sacral foramina. This should not be the case.
(There is a regular need for discussion in X-ray diagnostics, especially in the sacrum, and we are glad to have the support of CT and other procedures. In this so-called “polytrauma”, CT is particularly important as it clarifies further problems very quickly, as in this case: spleen injury, free air and blood in the abdomen, lung injury, blood in the thorax…..
The problem with the X-ray of the sacrum was pointed out in another article. “Loss of foramina, osteolysis in the sacrum on the right”
The fractures have healed well in the meantime. The patient suffered from bladder and rectal problems for a long time. He consoled himself – as he often did in life – “It could have been much worse”.
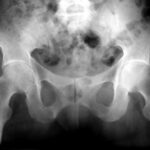
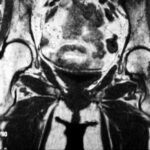
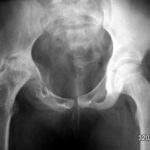
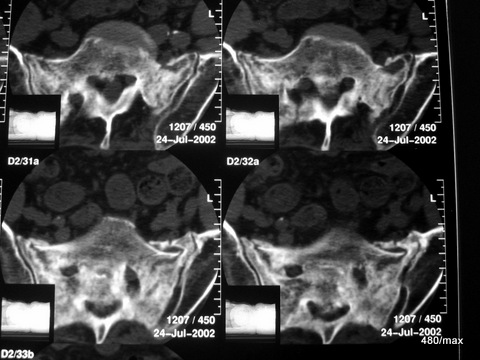
43 / 80 y.o. female patient. Osteomalacia with chronic fractures in the sacrum
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
Same method, same affected region, but no accident.
Extensive remodelling processes in both lateral masses. Vitamin D deficiency: osteomalacia.
The patient was in pain and ill at the time of this examination. She had previously helped out with her sick (adult) children in the business. Hard, unfamiliar work. The improvement she experienced after a few weeks of therapy was remarkable. –
The picture shows a clear difference compared to the last patient; here there is a smoothing and rounding of the fractures and a diffuse (blurred) compression of the bone. The healing forces are at work at the same time as the destructive forces.
44 / Turner syndrome, growth plates open for a long time.
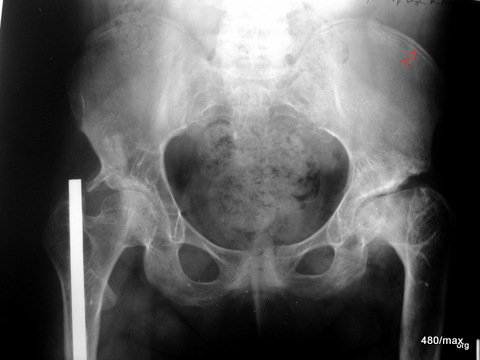
44 Where is the boundary between a growing and an adult skeleton? There are complex constellations in which a delayed closure of the growth plates occurs. We would therefore have difficulty determining whether we expect the sensitivity of a growing or adult skeleton.
Let’s take a leap backwards into adolescence:
This patient is 30 years old, but still has open growth plates like an adolescent; see pelvic scoop (red arrowheads). She has no current or recognisable chronic trauma. But she is in pain.
She has undergone several surgical procedures on both sides due to hip dysplasia. This makes it even more difficult to classify her in our scheme.
She has Turner syndrome, characterised by short stature and the absence of menstruation.
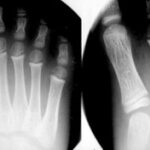
45 / Forefoot right: Tilt to view the growth plates, no pathological findings.
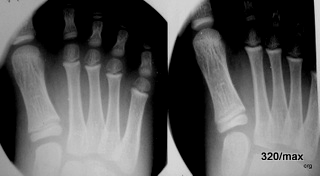
45 The image is for discussion of the projections only. Growth plates are not always visible in the radiograph. It is difficult, for example, if you do not have a parallel view.
8 year old boy. Tilting the beam path (right) provides a better view of the growth plates on the distal metacarpals, the metatarsals,
left: 25° and right 35° tilted X-ray beam (ventral/distal to dorsal/proximal). Does this have any significance? Yes, for example in the discussion about Köhler II disease.
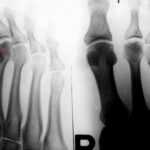
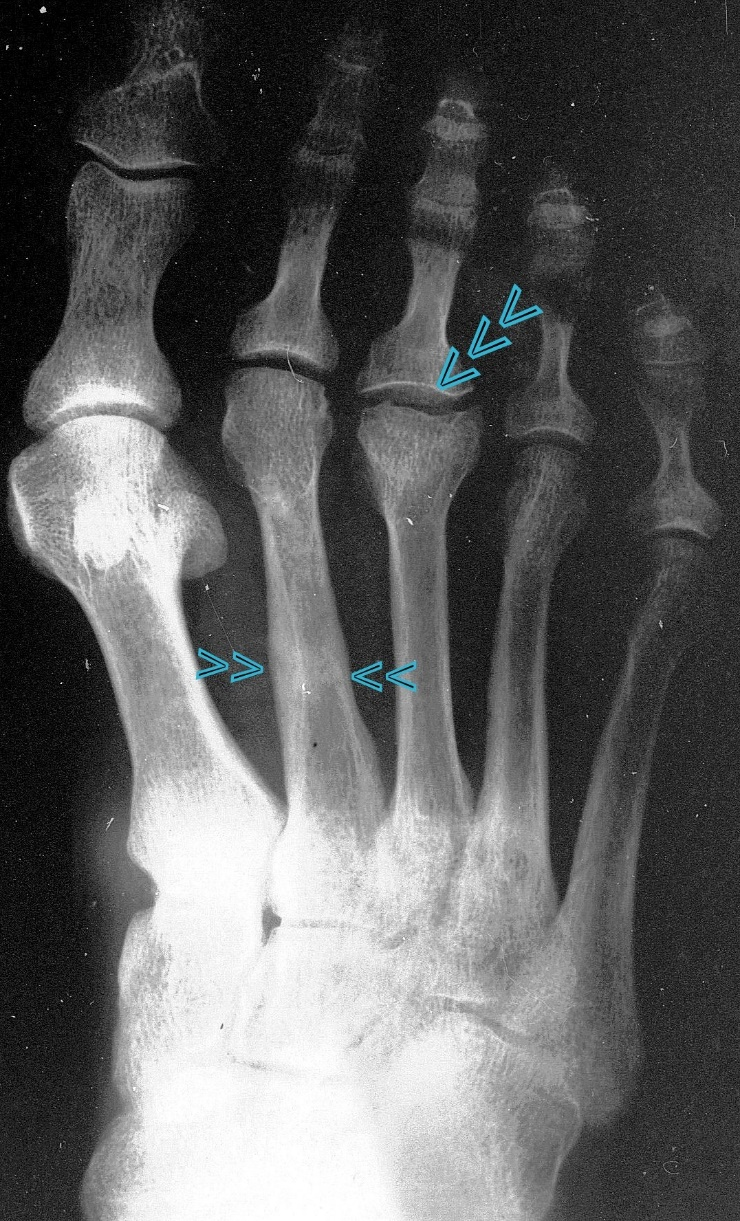
46 / Stress fracture in the shaft of metatarsal II + old Köhler’s disease II in metatarsal III;
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
42 y. male. X-ray of the metatarsus.
We know nothing conclusive about the history in adolescence. Current: 4 weeks ago unusual walking; hours later pain in the metatarsus and a circumscribed swelling: overload in the shaft of the metatarsal bone.
In addition something from a long time ago: Köhler’s disease II in the head III: all we see of the latter is an arthrotic residue of a disease suffered in adolescence in the growth plate/core complex of the head and the metaphysis close to the growth plate.
In the shaft of the metetasal II, a blurred line of compaction, partially lightened; apparently a remodelling process as in a stress fracture in adulthood.
The combination of a “Köhler II disease” with a stress fracture in the shaft area that is probably no longer fresh is interesting!
The message of this case is clear: same region (here metatarsus/forefoot) but certain differences, depending on whether the growing or the adult bone is affected.
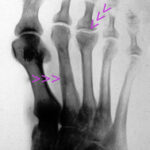
47 / Healing of a discrete Köhler II disease.
| Akutes Trauma | damals im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
The deformation in the head of the second metatarsal bone in relation to the joint surface is an arthrotic residual condition of a Köhler II disease that occurred during childhood. Many people claim to have observed this Köhler II disease at the stage of its development, i.e. in childhood. I have not yet seen any convincing pictures, especially not an observation of the progression (Alban Köhler from Wiesbaden will certainly have had suitable documents).
I do not want to claim that anyone is telling an untruth, only that a document proving this has not yet reached me. I would understand a complete observation to mean The stage of the first growth disturbances in the nucleus, possibly its displacement as an expression of damage to the growth zone, the reactions in the metaphysis with decalcification. Finally, the entire course of reparation with adaptation of the maturing nucleus and the resulting damage in the metacarpal head.
All the images I can find are arthrotic residual states of a disease suffered during growth. Theories on the development and surgical procedures are described.
With regard to the development, a simple solution should be added to the plethora of theories: an imbalance between load and resilience probably plays a (decisive) role in a vulnerable phase of growth.
48 / 65 y.o. man, lost his way in the woods and had to walk an unusually long way to find his way home. Metatarsal overload. MR
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
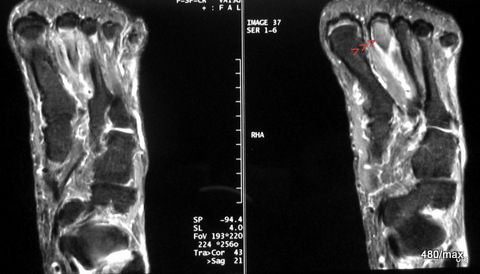
MR (STIR): Oedema (accumulation of water) in the heads of the second metatarsals II. The oedema is also in the shank (only a small section shown here) and apparently continues into the head. The history (and the rapid improvement with rest) leads to the diagnosis of an overload reaction.
We learn from this that chronic trauma in old age need not be limited to the shaft of the bone. It is quite possible that the change extends from the shaft to the diaphyses (the two ends of the growing bone in the area of the former growth plates). The fact that the head is involved is not a violation of the rules.
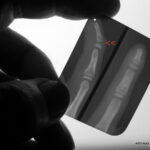
49 / 35 y. Doctor. Crash as cyclist with both arms over handlebars
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
49. pain in the carpus on both sides.
Contusion in the trapezium (one of the carpal bones) on both sides.
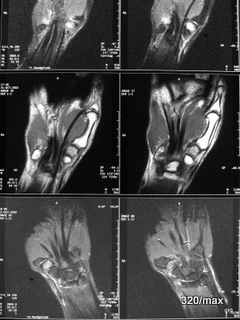
I have not made it easy for the reader with the MR images. You will recognise that both hands are shown. It is difficult to orientate yourself: STIR at the top and bottom,
in the middle T1.
Classic rules: In the STIR, all healthy bones are dark, the injured trapezium is light.
In T1, the healthy bone is intensely light,
the injured trapezium is darker.
If you have any questions, please write to me, dear reader.
The bilateral nature of the disease makes it interesting. Stress can act on one or both sides. Bilateral injury is something logical. If you look for bilateral injury, you will find it (bilateral injury is found in acute injury, osteomalacia and aseptic necrosis).
Forget – as already mentioned – the “Milkman syndrome”! “This American author (1930, 1934) published his report of a case with multiple spontaneous idiopathic symmetrical pseudo-fractures. Although aware that Looser (1920) had described comparable bony lesions”…..” (Google 20.2.23). The fact that a symmetrical Looser’s remodelling zone can occur is in no way surprising when one considers that all these disorders are basically overloads.
The syndrome mentioned is cited with overzealousness. The author Milkman would certainly be embarrassed. His publication does not contain a discovery, but a case report that confirms the observations of the Swiss Looser.
50 / child. Growth plate of the finger (end phalanx) blown up.
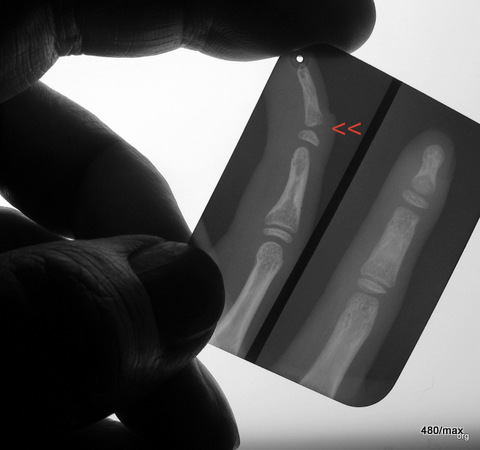
| Akutes Trauma | damals im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
If this finger is not treated well, it will not heal properly, i.e. with deformity,
Presenting such a tiny X-ray image is of course provocative.
I am showing it as a curiosity and historical document
from 1946; it is a “dental film”. It was also neatly “split in two”. The fact that it was necessary to save money back then – even more so than today – has been forgotten. (Another method of saving was “paper films”. They required a higher dose than the transparent films and were difficult to process (drying).
51 / Young adult; X-ray elbow: Avulsion of the ulnar epicondyle
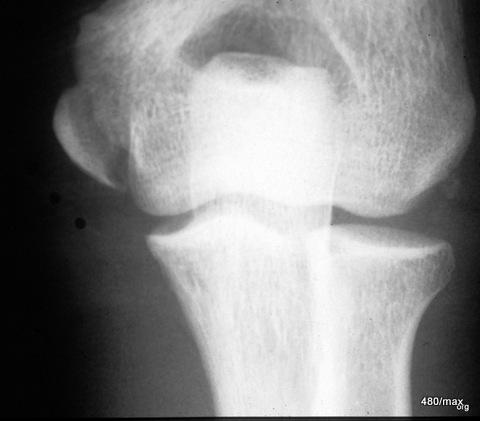
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
51 Several muscles (flexors on the forearm) originate from the epicondyle on the medial humerus (on the side where the ulna is located). For a more precise diagnosis, at least one further projection would have been necessary, possibly with comparison of the opposite side.
Despite the incomplete reduction, the consolidation was stable. It healed with good function.
52 / X-ray elbow. Patient with incomplete growth

| Akutes Trauma | im Wachstum | gesund. Kn. Weicht? |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
52. avulsion of the apophysis together with a piece of the underlying bone (the metaphysis). The apophysis is the bony core of the epicondyle. (You can still see the rest of the growth plate on the radial head).
It is somewhat complicated:
Apophyses (bony protrusions where tendons and ligaments attach) grow like epiphyses (the ends of bones close to joints during growth). In the joints, a growth nucleus is called an epiphyseal nucleus, and an analogous form of injury to the growth plate is called an “Aitken I fracture”, occasionally also referred to as osteo-epiphysiolysis/osteo-apophysiolysis.
53 / paediatric avulsion of the medial epicondyle of the distal humerus including a large part of the growth plate
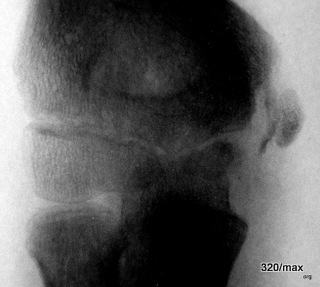
| Akutes Trauma | im Wachstum | gesund. Kn. Weicht? |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
53 Almost the same again with a much younger child. You should memorise these injuries and also the fact that there are such exceptions. This is a possible, but not the typical form of juvenile growth plate injury. Surprisingly, at least part of the growth plate has survived. More frequently, the growth plate ruptures completely in the sense of “Aitken 0”.
It is difficult to establish rigid rules for such a trauma in the area of the (former) growth plate.
Conclusion: Special attention must be paid to this problem region – the growth plate – otherwise you will cause serious growth disturbances.
54 / MR of a radial head fracture
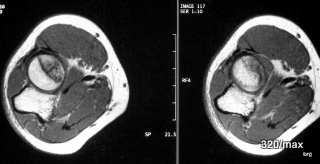
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
54. radial capitulum (capitulum radii) – Meisel fracture .
Conventional X-ray is completely sufficient in many cases, provided that a few tricks are mastered. See artefacts III, chapter 7, case 08. In this patient, MR is shown instead of X-ray, namely T1 weighted in axial slice guidance.
Normally, the circular disc of the radial head is uniformly bright. This is due to the abundance of fatty tissue. Here, this fatty tissue component is displaced by the fracture lines (surfaces) and accompanying haemorrhage and is therefore dark.
CT is also well suited to this issue. It is a faster examination than MR. However, positioning the elbow is somewhat more difficult. You can see the bone extremely well in the CT scan, but the bone marrow and some other soft tissues are not captured quite as well. –
Overall, the patient’s symptoms must be observed very carefully. If pronation and/or suppination are severely restricted and/or painful, special attention must be paid to the radial head!
To detect the fracture, you should use the method that you know very well. H.G. Schmitt proposed an X-ray method, used it throughout his working life and passed it on to his students. This had a high hit rate, especially in the case of less pronounced fractures: project the radial head freely (this is easy to understand)! Keep the device and arm immobile: only vary the pro/suppination 4 times, in 4 different positions of the radial head 4 very well displayed target names.
55 / Combination injury after Monteggia. Persistent dislocation after one year and accident admission
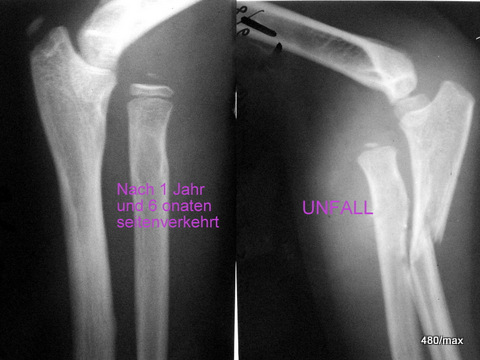
| Akutes Trauma | im Wachstum | gesund. Kn. Weicht? |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
55 I have collected Monteggia cases over a longer period of time and in different countries. Especially “overlooked diagnoses”. This has resulted in a large (and quite valuable) collection on the subject.
IN a picture section: elbow on the side after an accident. For those who are not yet familiar with the joints, it is important to remember this: The axis of this radius does not meet the small humeral head (capitulum humeri)! Alarm! Dislocation!
Other image section one year later: Unchanged dislocation! Malpractice! By the way, isn’t it remarkable how the growth nucleus of the radius has increased in size and shape; how a nucleus has also appeared on the olecranon (palpable elbow).
The most important information is that the radius is still dislocated. This must not happen! If calcification of the stretched capsule becomes visible, this is an additional indication that the capsule is under tension. It is so important that I would like to show another similar case.
With consistent further training, this misdiagnosis does not happen.
I assure you, dear visitors, that the last case was unfortunately not a “hummingbird”, not an unusual curiosity. It can happen to us every day.
To prove this, here is another case, 56:
56 / Second case of overlooked Monteggia; the combined injury 6 months ago! Here, too, the dislocation of the radial head was not recognised. This must be recognised (in the lateral elbow image).
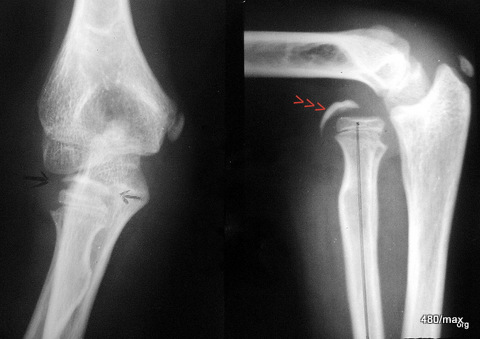
| Akutes Trauma | im Wachstum | gesund. Kn. Weicht? |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
56 The two images show the two planes at the same time, namely 6 months after the accident. The patient is youthful, but older than that of 55. He already has a well-developed nucleus in the radius, the neighbouring growth plate is already narrow; a sign that longitudinal growth will soon be completed here. However, the nucleus in the olecranon will continue to grow. The nuclei in the ulnar epicondyle and in the humeral capitulum (humerus near the joint) are also clearly visible. According to nature, the latter should articulate with the radial head.
But it does not: the axis of the radius drawn as a black line does not meet the centre of the humeral capitulum. This is a catastrophe!
The calcification in the capsule, which is already very clear here, is marked with black arrows and red arrowheads. The cause of the calcification is capsular stretching.
All readers are now familiar with the signs of dislocation of the radial head. If you are not yet familiar with the phenomenon of the calcifying joint capsule, this is a good opportunity to study it.
57 / 70 y.o. woman who slipped on wet leaves and fell on her buttocks. Old and fresh bony injury.
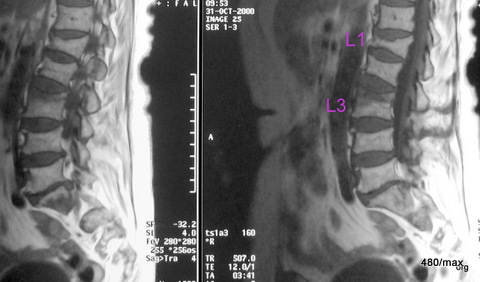
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
57 MR: two different sagittal slice images, both T1:
Old fracture L1 + fresh sintering L3. (L means lumbar spine). In the wedge-shaped deformed vertebral body L1, the signal is bright and even. This signal corresponds to a “normal” vertebra; only the shape is grossly altered.
In the upper part of vertebral body L3, on the other hand, fresh haemorrhage (perhaps already during the healing process) has displaced the fatty bone marrow. In other words, a change in the signal with (so far) little depression of the top plate. MR is a beneficial method here.
It is unfavourable to exaggerate the immobilisation therapeutically, for example by placing the patient in bed for weeks.
58 / Another leap back: to the adolescent skeleton. Growth plates in the forearm/wrist
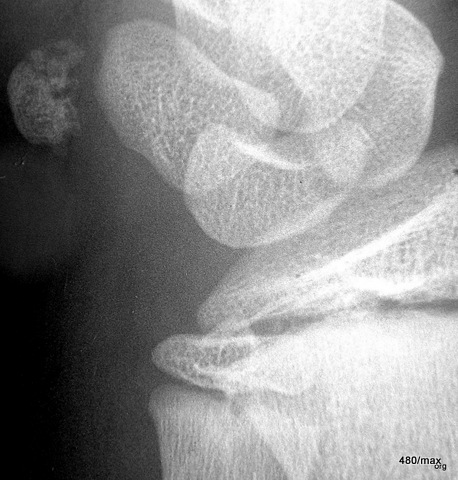
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
58 The above-mentioned growth plates are found in the ulna (lower left) and radius (lower right, partially cut off).after hard fencing training the boy has very severe pain in the wrist.
X-ray: Structural disorder in the pea bone (pisiform bone), a small bone of the carpus, which is embedded in a strong tendon as a sesamoid bone.
With this history and after ruling out other causes (infection, acute injury), this is suspicious of “aseptic necrosis”.
There are other sesamoid bones in humans. The largest is the kneecap. It can also develop aseptic necrosis (according to Larsen).
59 / Periarthritis humeroscapularis
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
59 Blue arrowheads are intended to mark the pathological calcifications. (The left group of arrows should move a little to the right).
In contrast to most of the cases of disease shown so far, this is a change that takes place in the soft tissue, more precisely in the capsule-ligament apparatus. The connection with chronic traumatisation has not been conclusively proven. An imbalance between stress and resilience is likely to play a role.
Osteochondrosis dissecans and joint chondromatosis have a similarly unclear relationship to stress .
I mention them in order to add the following to the discussion: Overuse injuries of any kind, can occur not only in bone, but also in cartilage, tendons, ligaments and muscles. All of this is one unit. Junghans first formulated this in relation to the spine: Do not consider bones and soft tissues on their own, but understand movement segments as functional units.
60 / Chondroma knee joint
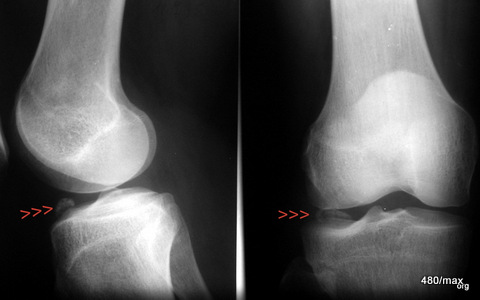
| Chronisches Trauma | Ausgewachsen | Disposition im Knorpel? |
60 In this rather rare cartilage disease, hyaline cartilage nodules (often with a calcified centre) develop in the joint space and in the synovium. Only one such formation is shown here and marked by red arrowheads. They behave like “joint mice” in osteochondrosis dissecans; however, a mouse bed is not detectable here. In joint chondromatosis, free cartilage nodules occur more frequently in larger numbers. The knee joint is less frequently affected than the shoulder, hip and elbow joints.
If there is a risk of such formations becoming trapped in the joint and damaging it (osteoarthritis), arthroscopy (or surgery) helps to remove these interfering bodies; the cartilage is protected.
The links with overload damage are unclear.
61 / Insufficiency – Fracture of the lateral masses of the sacrum (the lateral parts that are articulated to the pelvis).

| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
61. 56-year-old woman. Few of the cases of illness shown were so dramatic.
Not an accident. Cortisone (oral) for years for bronchial asthma and carbimazole for epilepsy. The patient had to work a lot due to a move; more than was permitted with her previous illnesses. Rapid onset of dramatic pain in the lower back. These were so severe that an advanced malignant disease was suspected.
The sacrum was affected, particularly its massae laterales. This section of bone consists of a delicate network of bone beams; the entire weight of the upper half of the body rests on it. The exit holes of the “sacral” nerves (S1-ca. 6) should not play a role in stability, as they lie deeper. The bone was pre-damaged; hence the term “insufficiency” fracture.
Time to draw special attention to “Osteopathia antiepileptika”. Practically the same is: “Osteomalacia with antiepileptic treatment”.
The first literature reports are from 1967! Schmid and Kruse two highly deserving authors. For further reading see: Marianne Vathar-Matiar + W. Fröscher: Osteopathia antiepileptica in adolescents and adults; further literature from Wolfgang Hetzel.
The clinically severe cases were observed with multiple combinations (barbiturates + carbimacol), long treatment duration, concomitant neurological diseases and in institutionalised patients (risk factors, so to speak). Vitamin D hypovitaminosis is very often the cause. This opens up a promising treatment route (1000 – 5000 IU Vit D). Sunlight and regular exercise are also helpful for prevention. With prolonged, high-dose Vit. D treatment, there is concern about accumulation: loss of appetite, vomiting, thirst and polyuria. Nephrolithiasis and extraosseous calcifications are mentioned. H.G. Schmitt, who diagnosed and treated many osteomalacia, saw these complications very rarely!
I no longer have the conventional X-ray image. According to my memory, nothing (?) was visible. I have already described how difficult the X-ray diagnosis of the sacrum can be.
In this case, it is much easier in the MR: STIR, T1 CM+, extensive oedema in the massae laterales of the sacrum. A strong “accumulation” after contrast medium indicates that the metabolism is intensively fuelled. This could be the case with a malignant disease, inflammation or trauma.
In our case, the localisation together with the history suggests chronic trauma.
MR or scintigram? A bone scintigram would also have been very useful, as it would have shown a massive accumulation of activity in the “massae laterales” and probably nothing else conspicuous in the rest of the skeleton. This would have been an argument against a malignant event, and together with the previous history, this argument would have carried a lot of weight. Overall, it must be emphasised that skeletal scintigraphy and magnetic resonance imaging (MRI) have significantly improved the diagnostic possibilities.
Despite the high probability of a benign disease, it was impossible to avoid looking for a malignant disease. Fortunately, this was unsuccessful. This saved the patient from having to have tissue removed from her sacrum.
The pain was managed with extensive immobilisation and vitamin D. I would say “quickly”; for the patient it took an eternity. The medication was carefully modified.
The following can be added to the medical history: the patient had been inadequately cared for for a long time with regard to her asthma and epilepsy. Good medical supervision would have recognised problems and weaknesses in the medication and taken countermeasures. Corticosteroids are important and often indispensable drugs, but you have to know the side effects very well, observe them and take countermeasures. The same applies to anti-epileptic drugs.
62 / Rear-end collision 6 weeks ago, pain in centre of sternum, increased when coughing
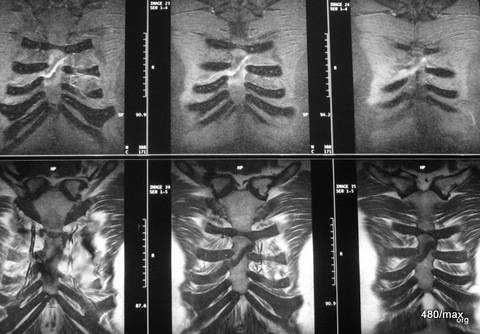
| Akutes Trauma | im Wachstum | gesunder Knochen |
| Chronisches Trauma | Ausgewachsen | kranker Knochen |
62. Der Patient hat sich den Humor bewahrt; er könne noch lachen, allerdings täte es ihm etwas weh. Auch die Entleerung des Darmes wäre eine schmerzhafte Aktion und ebenso das Aufstehen aus dem Liegen. –
Im Röntgenbild war die Fraktur fraglich. Man wunderte sich über die hartnäckigen, umschriebenen Schmerzen.
MR: Sternumfraktur, schrägverlaufend im Körper des Brustbeins, man möchte gerne noch eine sagittale Projektion sehen, um die Verschiebung nach vorne/hinten abzuschätzen. Eine grobe Verschiebung (Dislokation) bestand nicht; daher wurde das Bild weggelassen.
Die vorangegangene Röntgenuntersuchung hat einen Sinn gehabt: sie hat einen blutigen Erguss zwischen Brust- und Rippfell oder einen solchen im Mittelfeld (Mediastinum) recht gut ausgeschlossen. Auch der Pneumothorax war “vom Tisch”, besonders die gefährliche Form des “Spannungspneu”. Noch einige andere Diagnosen waren damals ausgeschlossen worden. Dabei hat auch der Ultraschall (Sonographie) mitgeholfen; man möchte diese wichtige Methode nicht nur am Bauch auch bei einer Verletzung des Thorax nicht missen.
MR: oben STIR und unten T1; gut geeignet um die Gewebe-Charakterisierung in der MR zu verstehen und zu rekapitulieren.
Im Frakturspalt (blutige?) Flüssigkeit hell in der STIR, dunkel in T1. Keine Reaktion in den benachbarten Weichteilen, ausgenommen im frakturnahen Knochen: am deutlichsten in der STIR.
War die MR in diesem Erkrankungsfall nötig? –
Bald bildeten sich die Schmerzen zurück. Der Patient traute sich wieder zu lachen. Es ist keine Stufe an der Oberfläche des Brustbeins zurückgeblieben.
63 / Cough fractures
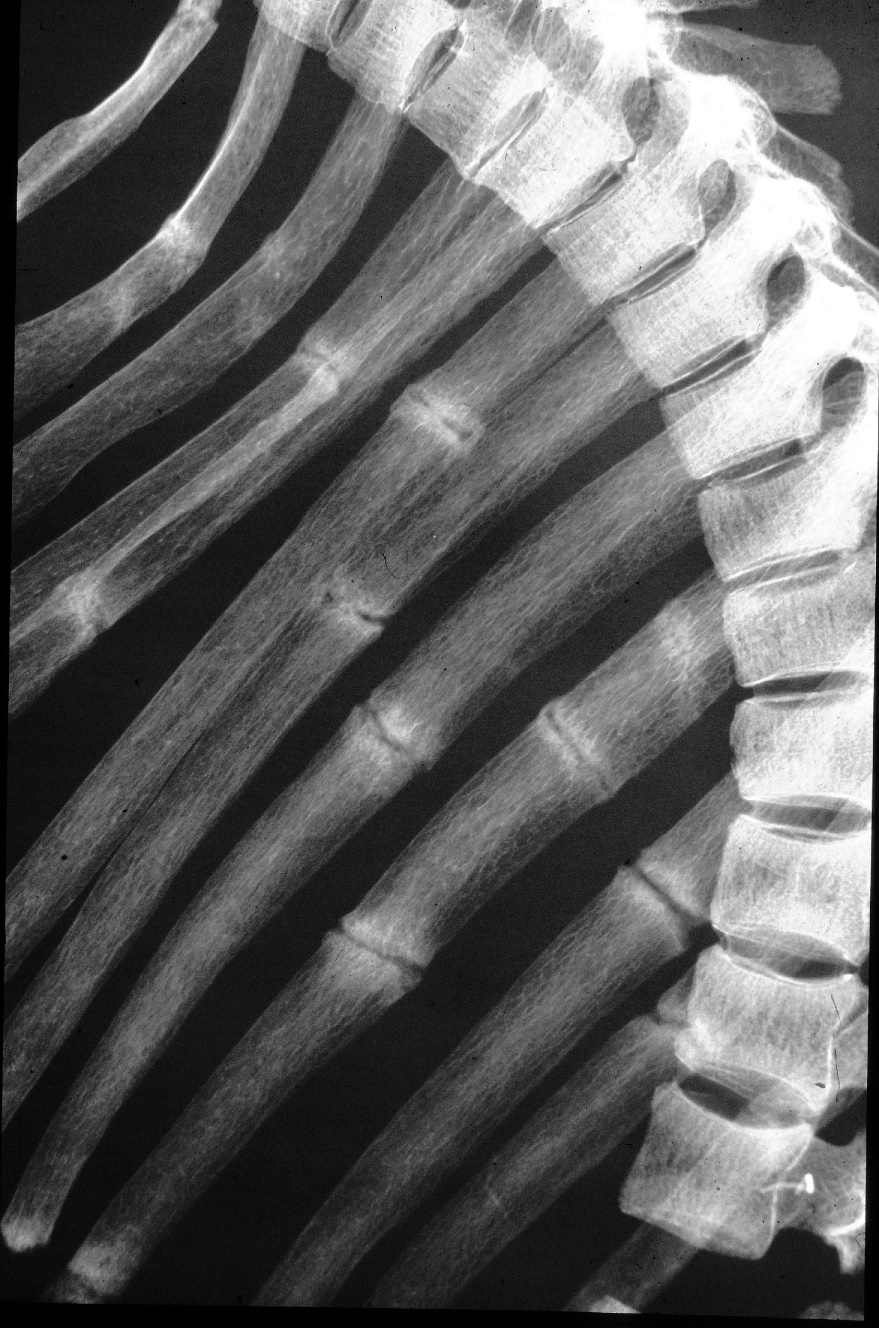
| Akutes Trauma | im Wachstum | gesunder Bandapparat? |
| Chronisches Trauma | Ausgewachsen | Vorschaden ? |
62 A seriously ill person with a bone metabolism disorder, probably specifically a vitamin D utilisation disorder. The ribs were not able to cope with the strain of a strong cough and reacted with overload zones. Characteristic are the uniform, relatively wide “fracture gaps” with strong compression (sclerosis) of the neighbouring bone. This picture was taken after death for a scientific reason. It was made by Prof E. Ühlinger after his death.
It was made by Prof E. Ühlinger. I keep the original. A good opportunity to commemorate a brilliant pathologist (and radiologist). He was a doctor and philanthropist; he was also committed to the victims of concentration camps. He co-edited Schinz’s textbook for many years. (H.R. Schinz was also Swiss and worked in Zurich.) Some of what E. Ühlinger said has been forgotten; some things were not fully understood. He had a talent for not overcomplicating things, but for looking for big connections and thus making many things understandable.
Everything can be sorted into closely neighbouring drawers: One drawer” is labelled: acute fractures.
And then there’s another drawer “Overload on adult but diseased bone” and 7 more.** You will notice that I also collect old pictures. (I have recently been focussing on the doctor and radiotherapist Carl Fried, Worms and Breslau, who was imprisoned by the Nazis in 1939 and was eventually able to flee to Brazil).
14.5.24