Cases 76-80 Paraffin plombage and/or oil plombage
14.11.25.
76. Paraffin plombage and/or oil plombage
are, in essence, residue formations of a long-forgotten type of tuberculosis treatment.
Both may be summarized as “oleothorax.”
The term “oleothorax” comprises all fat substances and is not restricted to merely “mineral or vegetable”oil.
First we see CT-slices and reconstructions of one single patient. Go through fast. You will realize later what the typical findings and what the exceptions are.
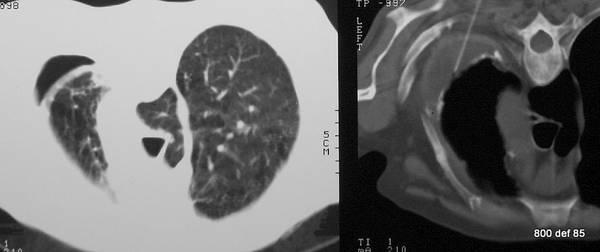
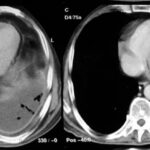
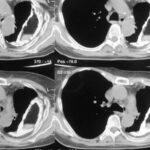
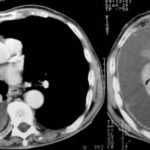
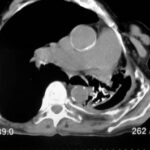
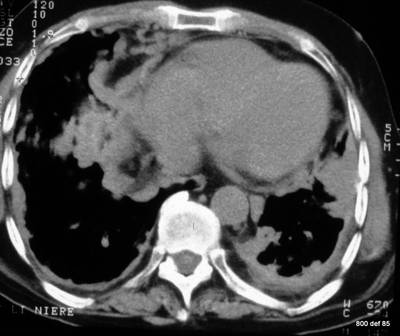
picture 76a – f : We start with the first patient with atypical plombages on both sides. a + b:
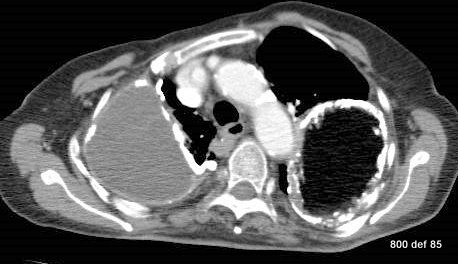

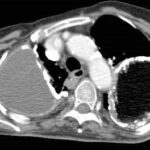
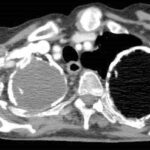
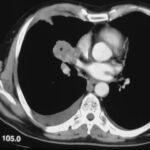
picture 76c: You admit it is plombage on both sides. oleothorax??
76c. If you don’t see any problem go on to case 93. Otherwise this case collection will help you to get familiar with the old formations of a tuberculosis treatement.
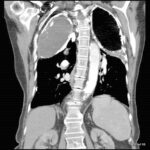
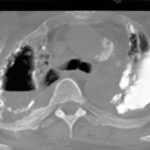
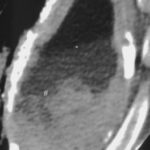
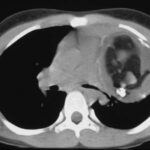
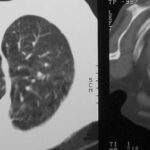
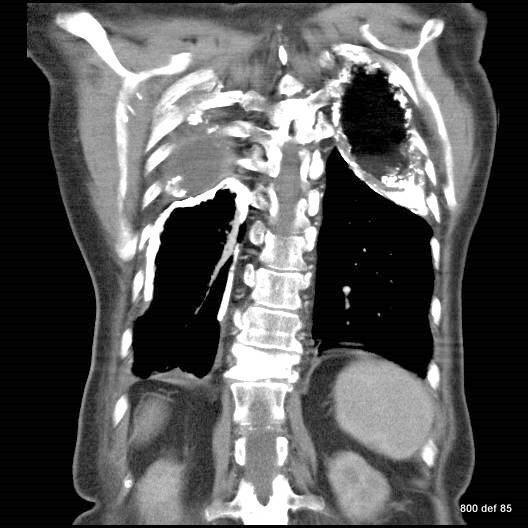
picture 76d: Sagittal reconstruction.
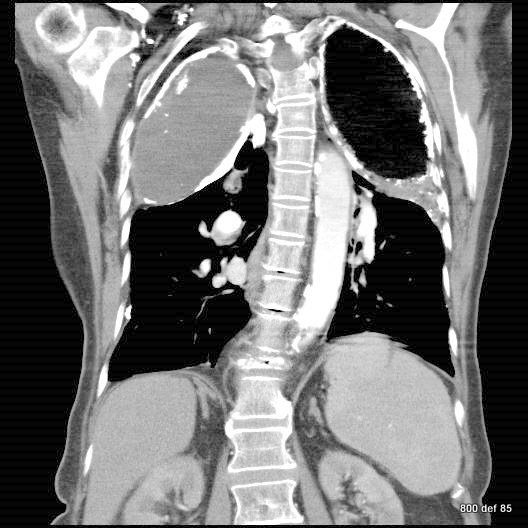
The first impression for a problem which is discussed later in detail.
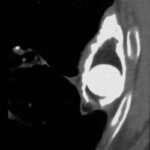
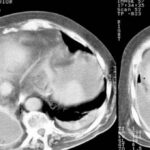
picture 76e: We will learn to differentiate between changes in the contents of plombage and in the wall.
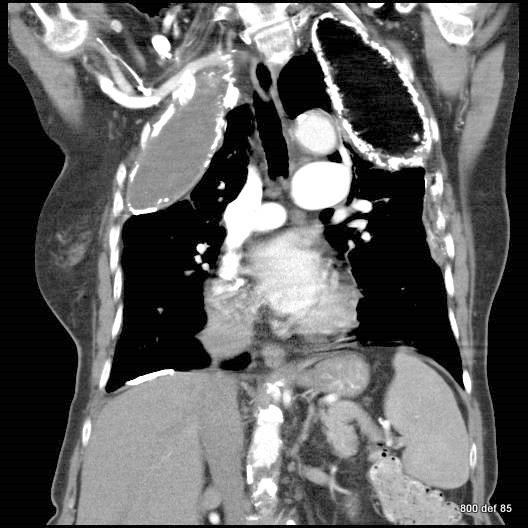
Plombage treatment was used in the second quarter of the 20th century.
Oleothorax belongs to the “collapse therapies” and how they were employed in serious to influential caverns of the apex and the upper fields.
What other collapse therapy forms were once in use?
There was once additionally
– the pneumothorax-therapy as well as
– the thoracoplasty.
The Hein-Kremer-Schmidt book from 1938 provides information about collapse-therapies in lung tuberculosis in the wider Eurpoean field and area. The three parts of this weighty and well-informed handbook deals with the three so-called “collapse therapies” and their benefits as well as their drawbacks. In the USA, it is dealt with in Alexander’s “Monography.”
The advantages of oleothorax in comparison with pneumothorax was the unique operation itself. (The air of the pneumothorax had to be renewed quite regularly after some weeks, or indeed after some months).
The advantage of oleothorax vis-a-vis thoracoplasty was the much less serious operation, which did not require the ‘resection” of several ribs.
Why must we still recognise these pictures and images today ?
Even today, we may see these thorax results ; What is so important is the detailed knowledge of the various complications: they are rarer than during the long-time observation of the “Light III empyema” (see our cases 45 –75).
A small remnant concerning the DD oleothorax- chron.empyema. Sex differentiation maybe ? During the oleothorax observation of Obert and Schmitt, 8 women and 4 men were involved; during the empyema-residual predominantly more men than women were involved.
Anamnesis and X-rays make the diagnosis simple. What is important for the radiographs is as follows: these oleothoraces have become calcified on the surface area after so many decades. These images actually belong to the differential diagnosis of the calcified thorax shaded regions.
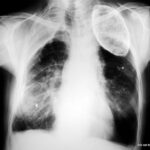
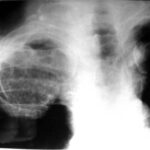
We did a special way through the patients imaging; we end it with the ordinary chest x-ray; a lot of special findings from the CT is not visble, but the knowledge of CT is an advantage for us.
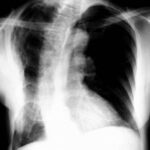
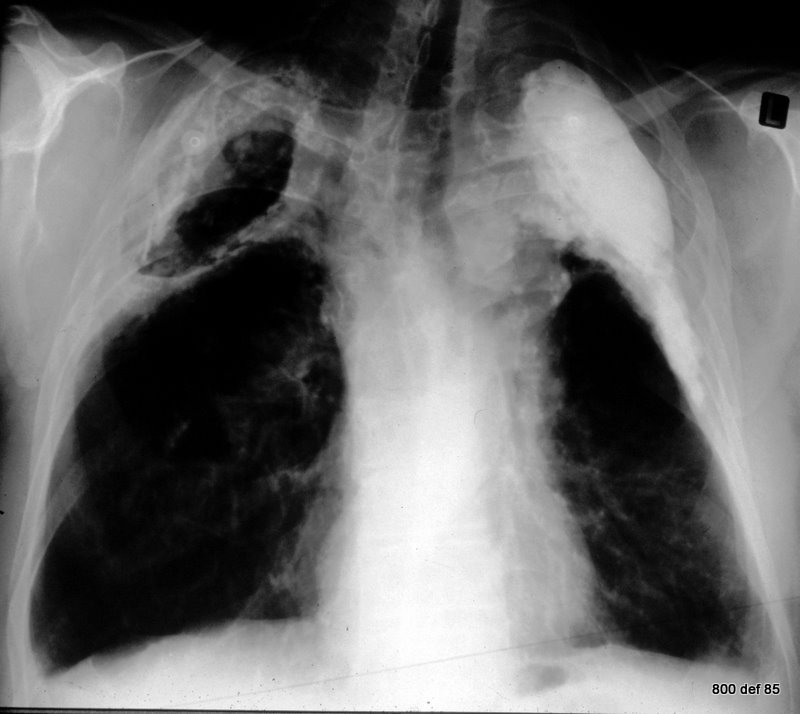
picture 76f; New patient: The x-ray summarizes the findings. What is your diagnosis in the right middle/lower area of lung (maked with a #) ?
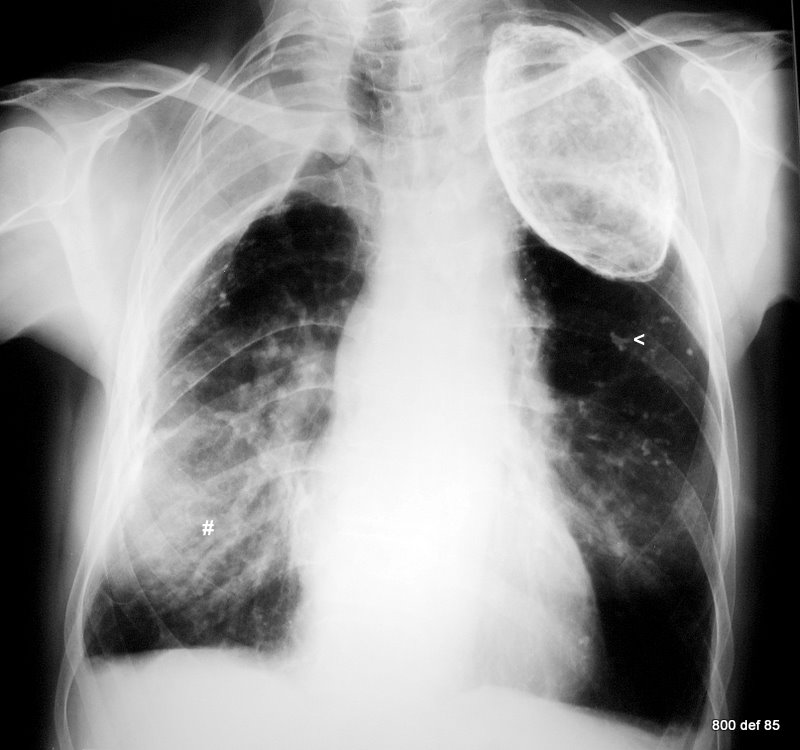
Check the so-called opinions as regards this particular thorax images. How reliable are they?
1.The wall calcification is (on the right) typically thin: on the left, uniform and thick. Finding Number 1 has so many exceptions that one really must discuss them in order to reject or dismiss any of them
2. The uncalcified layer between Calc. and the inner thoracic wall is thin: the thinner part is to be found in chronical empyema (Light III , see case 40-75).
3. From the shape, it could be (right) – oil, and (left) paraffin. It certainly accords fully with the history.
Take especial note of the thick-calcified residues in both lung areas, the calcified pleura-skin in the right middle area. This continues towards the dorsal area and simulates the shading of the right lung middle/lower area (#).
We must discuss an anatomic detail more specifically.picture 77:
Pic. 77: New, Two different cases; x-ray
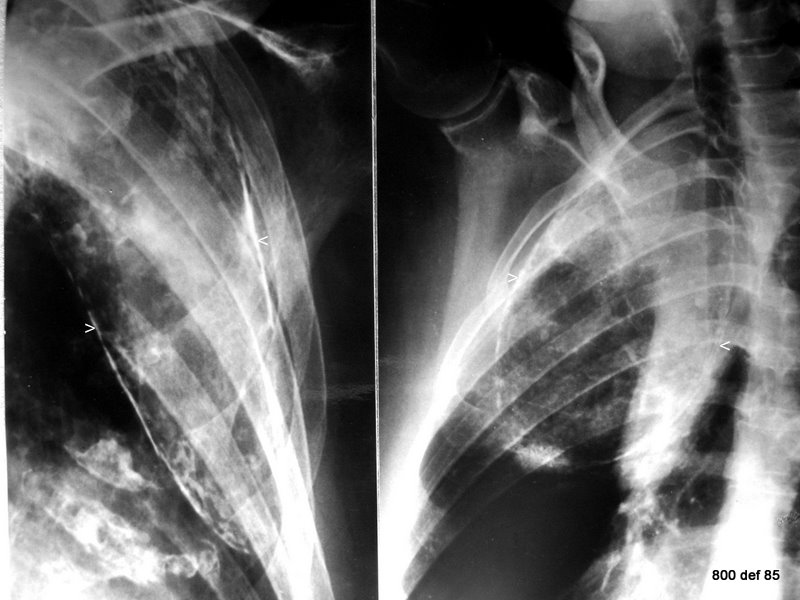
The female patient on the left had therapy for cavernous tuberculosis of the lung at the age of 47; she underwent plombage with Paraffinum (in Europe the preferred material)- X-ray examination took place at the age of 91.
Patient right received an oleothorax aged 32. This X-ray dates approximately 45 years after. –
It is probable that oil was employed in this case.
Both cases are typical;
the Findings 1-3 may be confirmed in both cases. Please relate the photographs in a very good light .
Anatomically-speaking, where precisely is this fatty material introduced?
It is especially important to know that these foreign -body objects material are located extrapleural,
that is to say,
are introduced between the thorax wall (Fascia endothoracica) and the Pleura parietalis. The foreign material is not to be found within the pleural space itself.
Complications may be caused by dislocation into the pleural space. This dislocation (in addition) ruins the therapeutic effect.
In fact, in the initial phase of this therapy, one started trials and tests so as to provide substance to the pleura space itself. This was an artificial effusion with fat or oil. The method was forsaken in favour of extrapleural plombage. In The USA, this was seemingly not a strict rule.
In America, it seems actually to be the case whereby, in addition to the extra-pleural area, the regular pleural space is used quite extensively. At least 3 US authors from the time-frame pre-1950s (i.e. Witnesses of that period in history ) position the intra as well as the extra-pleural plombage, both with equal rights and emphasis, side by side.
Hutton (1983) and Deboisblanc (1988) both state and cite this very fact.
As far as the intrapleural method is concerned, oil was the substance of choice (Deboisblanc).
Concerning access to the intrapleural area, there was a far larger incidence of complications compared to the European recorded annals, and so was recorded the result that oil should, as best as possible, be once again removed.
It could well be, that this caused or resulted from a misunderstanding.
The truth is, that the intrapleural application represented merely an exception. Would the intrapleural access always, time and time again, be quoted , although it was the exception to this rule ? – –
Literature also sees the juxtapositioning of paraffin and oil. The commonly-held definition tends to promote or further misunderstanding due to the lack of sufficient knowledge. The incorrect opinion: “Oleothorax means – apodictically – the employment of oil”. Many authors hold, quite mistakenly, this ill-advised..
The complete definition runs as follows: oleothoax is the introduction of fatty substances. Paraffin or oil: oleothorax does not exclude paraffin.
From the many substances, with which one has conducted experiments, it is the paraffin-oil that contains the fewest complications. Paraffin may be slightly warmed (and thereby rendered fluid) and introduced into the surgically-modelled space and then retained tight or semitight at body temperature.
This holds good for the European field as well as for certain American authors. J. Alexander (1937) prefers the extrapleural pneumolysis. And it is here that the favourable characteristics of paraffin may be witnessed. It is from Alexander and from Hein, that the two important monographs emanate.
picture 78: CT of a new patient with a pace-maker. Fibrousing of the pleura in the left upper area after a specific process. Paraffin plombage in the right top upper area.
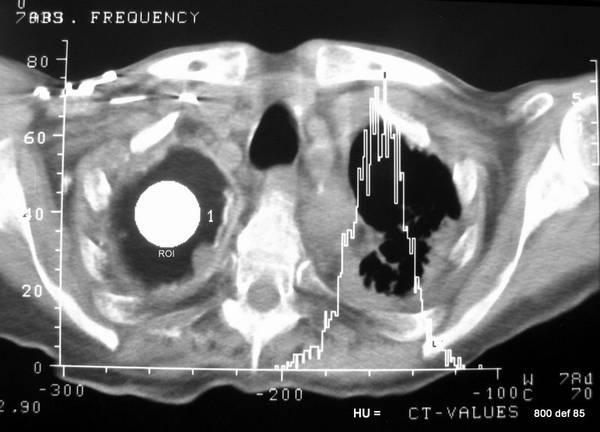
A “Histogram”has shown for a so-called “region of interest (ROI 1 : depicted as a circular white area). What precisely is a histogram?
Frequency distribution vis-a-vis CT values (= Hounsfield Units = HU) of the volume-elements. Two values are true representatives of this frequency distribution.
Mean = – 160 HU . Whereby the standard deviation is 15 HU.
CT values of paraffin are, therefore, still below or less than fat tissues.
The cavern content is rather darker than the fat cells.
It is simple to understand: to be found in the fatty tissue are also cells (egg white, containing water, approx 50 HU) and not merely fat, as to be found in one such lead substance. A fat cell has accordingly higher HU than this mere fat.
Incidentally, the calcification here is only partially pronounced.
Picture 79: A new patient. Unusually dense substance in the left upper area, with a similar density to Compacta of bone. Content of the right-hand side plombage has been coughed up due to a conection to the bronchial system.
79. Are there plombages with other materials and combinations, rather than with paraffin or oil ? In this new case, what precisely is the plombage content both on the left and the right?
It is quite apparent that one has done many experiments. The main point however: the substance introduced to compression was easily digestible. So, no surprises at all that we may come across, as an exception, other materials, too.
An unusually dense substance is employed in the left upper area, approx +1000 HU. The reason behind this very highthickness is due, quite likely, to the fact that the oliy / fatty substance was added with iodine salt content. (The same in 76 a-d !)
It is quite often mentioned in literature that Gomenol/ Gomonol , an extract from the myrtle tree leaves, is added. The frequency of this mention does not, however, necessarily accord with the significance or meaning. – The effects of this or other additives to the radiation absorption have not been investigated.
Because the left-hand side plombage is a little elyptoid or spherical and extends further caudal, that is why the content is probably liquid (see finding 3).
The thickness of the soft tissue layer between the plombage and the inner wall of the thorax is remarcable.
On the right, the plombage wall is unusually thick; the calcification there is quite irregular.
The content of the right-hand side plombage has been coughed up due to a complication (here, a pleuro-bronchial fistula) so, we find air in this artificially-manufactured extrapleural space:
the description as “Pneumothorax” is partly right and partially wrong. One should, therefore, really try to avoid it.
Lengthy, formed structures, which melt with warmth, appear in the sputum area with such fistulas. The paper of Wood calls these ” wax-worms.”
The relative density of the layering between the plombage and the thorax inner wall is remarkable, usually we find fatty tissue in this layer.
Case 79 is similar to case 76 a-e. Just the same two (very rare) findings but on different sides. We should not loose observations like that. CT follows in 80.
Picture 80: CT of the patient in 79.Very much simpler using CT. Indirect signs of a fistula formation right side..

What may be found in the right side of the “Blombage area” ?
– Air, above the liquid surface.
– Liquid under the surface: after the CT-values, this could be a protein rich fluid (exsudat).
We do not know when precisely this exsudat originates. Has it its origin (inflammatory mobilization with or without super-infection). Did it already appeare before the fistula and then continued thereafter ?
As to the complications:
An earlier complication:
– The plombage can rarely provoke mechanical alterations: upper influx blockages and build-ups, as well as thrombosis of the jugular vein or of the subclavia.
Complications after a few years:
– we have already identified the simplest and the most common complication: namely, the foreign-body reaction of the cavernous wall (accompanied, over the years, by calcification deposits). This fatty material is – because of the period length- not so inert, as hoped. This complication is to be found in almost all the patients.
– Quite a common reaction is the sterile or infected exsudat-formation in the plombage. This can lead to a perforation.
-I observed, upon two occasions, a fistula from oleothorax to the bronchial system. The fluid, oily substances can cause Alveolitis or so-called mineral-oil-pneumonia.
-Regarding a perforation, the oily mass can also reach to the mediastinum (causing so called “Paraffinomata”).
-The further onset of an “exsudat-granulomatosa-Perikarditis”is very rare.
Haberkorn (1989) reported about the possibility of a ray – induced malignant tumour. In addition, in Meyniard (1980) ‘s document, we may read about a ” foreign-body sarcoma.”
One may easily conceive how pathogens can achieve secondary penetration in to the vacated plombage capsule. This is given that there is not already, before that penetration, some form of infection, which caused that very penetration. Both can be described as being, “cause and effect.”
Cases 81-85 Early and late complications
Picture 81: A new patient
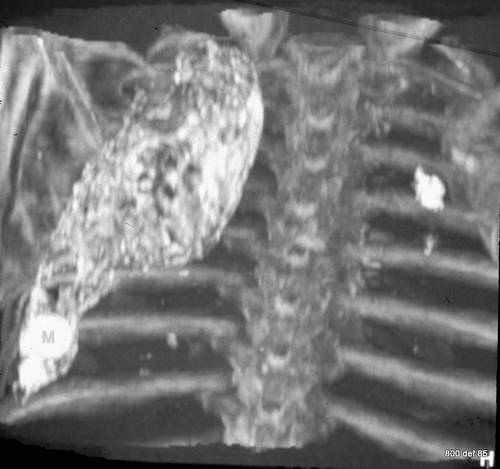
Which technology?
Maximum-intensity-projection: in this way, a larger number of CT slices is totalled up. This addition concerns merely the densest image-points, so that bones, chalk (calcium) and various contrast agents are stressed.
We may see a large plombage with an irregular calcified wall. The shape shows us that the plombage content is oily, i.e. Fluid and not solid. The Densitometry permits an unambiguous diagnosis of the oleothorax, but is unable to properly differentiate between oil and paraffin.
A thick, spherically rounded formation is to be found in the caudal section of the plombage. In the case of a fluid content, these bodies may move freely = i.e. Dipping down to the lowest spot.
Karl Gürtler MD (Bielefeld/Germany) described such a “Plombage Mouse”and documented this incident from different angles and positions by means of fluroscopy.
82. Strong and significant irregular wall calcification.
Oil is a little less dense as fat cells, but significantly denser than air: quite typical, therefore, for an oleothorax.
Within the plombage itself may be found the already-described , spherically rounded, homogen-calcified image: a “Plombage mouse”
Picture 82: Patient already displayed in 81. CT- transversal cut – in the lower part of this plombage.
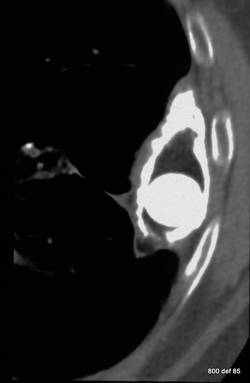
83.Installation of a plombage in 1939 cause of a therapy-resistant, open lung tuberculosis in the left upper region.
picture 83. What is typical? What is not totally normal? What known complication has already commenced?
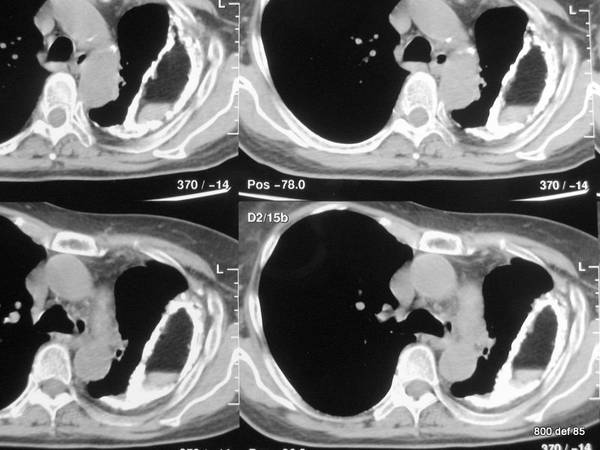
First of all, we shall document what is typical: foreign-bodies’ reaction to the wall leading to calcification: a complication which occurs regularly after several years.
What is noteworthy in some cases is the shrinking of the left thorax with all of the inherent signs:
– This expiration posture is typical for a shrinking process.
– Diminishing and reducing “intercostal spaces” (only a swelling and thickening of the ribs is not yet proven).
This shrinkage is atypicaly for oleothorax; it is much more common in fibrithorax (with or without chronical empyema). We suppose the shrinkage is a result of primary toberculous infection and nor a complication of therapy.
84. Same case.
Another uncommon but typical complication is:
Exsudat influx in the plombage content. (Hutton, 1983; Mullin,1986)
picture 84: Remark the mirror between fat above and exsudat below.
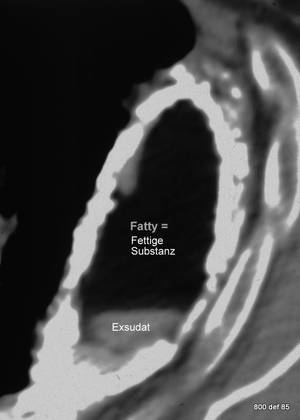
To repeate: which additional and rare complications are not detectable here as a threat, but are here as part of this combination ?
The rare plombage perforation
– in the soft areas*
– in the bronchial system** (Mullin 1986 , Tsou 1978)
– in the mediastinum (Deck 1969)
– the rare infection case
*Pleurocutane Fistula is described by Howlett (1937) and by Hayes (1933) . (see our patient Nr. 74 in paper 06)
** Twersky (1972) observed a post-traumatic , provoked fistula.
85. Further oleothorax with Paraffin.
The commonplace, reactionary wall-thickening is very clear. The calcification tends to be especially thick .
picture 85: The inner regions of the caverns show there to be a three-layered structure
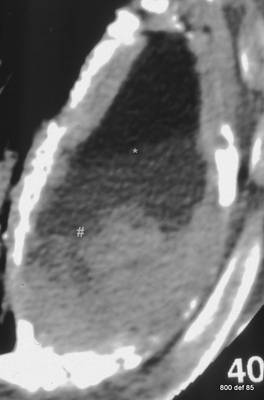
What, in all likelihood, are the pertinent composite parts in this formation?
Top: fat (-80HU)
Middle: exsudat (+15HU)
Bottom: exsudat with cell-damage (+45HU)
At the time of the examination, there was no clinical proof or evidence of an infection.
Cases 87-90 Empyema necessitatis, Thoracopasty (combined with a dislocated plombage)
86. I wepeat this case: 30 years after installation of the plombage
picture 86: What complications might arise 30 years after the installation ?
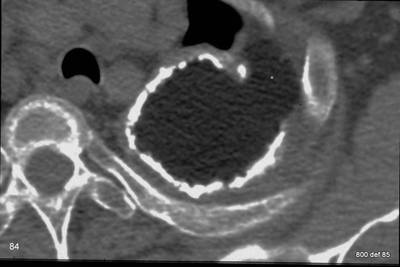
Paraffin is worn down at a small point in the space between plombage and a rib.
picture 87 : A new case of a very elderly patient. – At the age of 50, he survived a lon-term tuberculosis and the full procedure of surgical treatment
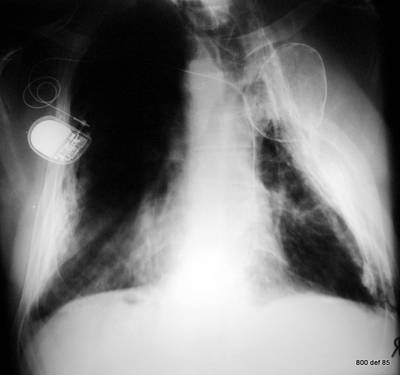
What mistakes and what peculiarity does the thorax shot of ?
On his left thorax, the patient has an extended thoracoplasty and a small, additional oleothorax . The plombage is dislocated and may, thereby, have lost its effectiveness.
This combination of ‘methods for therapy-collapse” is exceptional. Nowadays, we do not acknowledge the peculiarity of this illness case, which gives cause for this broken-down combination of a therapeutic procedure.
88. CT of the same patient (87).
Picture 88 : CT of this Thoracopasty combined with a dislocated paraffin plombage.
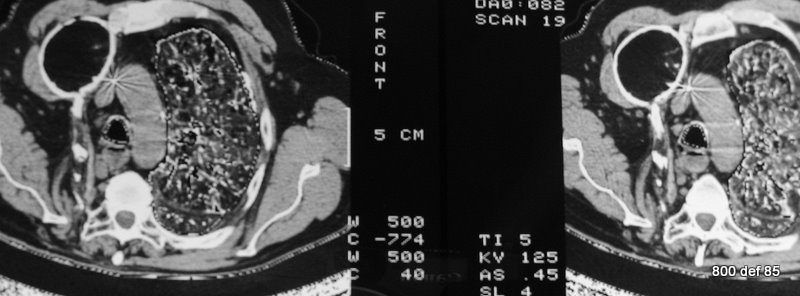
What technical peculiarity does the image of the left lung show us?
A “double window”; the soft-tissue-area, as well as the lungs should be well depicted in one picture. This window is not readily showed any more!
89. Today, we have little practice with the assessment of thoracoplasty.
For that reason, we would rather like to study – using three subsequent cases – the complex effectiveness of the entire bone, comprising thorax as well as of the spinal column.
Picture 89: Thoracopasty; study the effect on ribs, spine, diaphragm
So, here, why has one not employed the plombage, but far rather the comparatively complicated operation of the thorakoplasty?
One can imagine that the cavernous process was loctaed, rather than in the upper regions, in the right-middle areas. Such localisation was “laid to rest” poorly by the plombage.
It is not easy to decide: are the ribs rarified and ill-formed , or is the soft-area-coating “diffus” calcified and ossified (see 92).
Picture 90: A further case of thoracoplasty
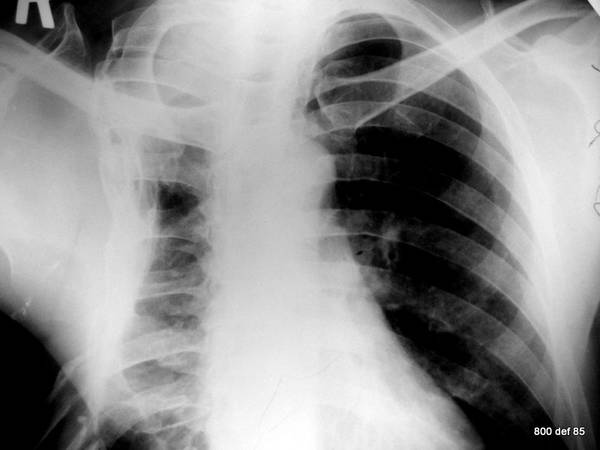
In order to conduct further studies of the operating method, one has to turn to two old-fashioned publications for advice and counsel: Hein-Kremer-Schmidt (Collapse-Therapy and Tuberculosis of the lungs) and Alexander’s textbook.
Picture 91: A further case of (a left-side) thoracoplasty
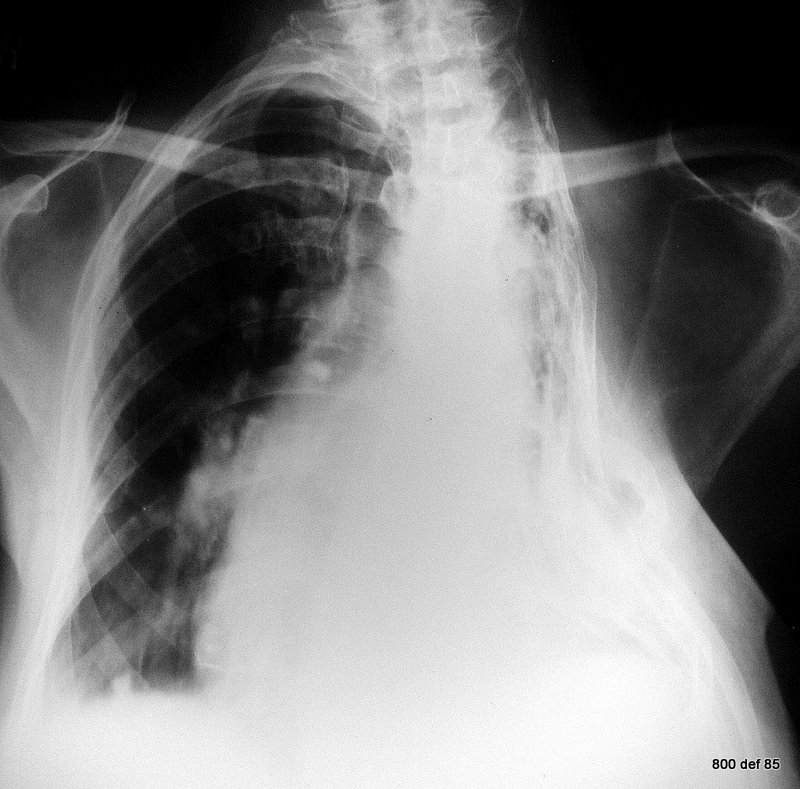
These operations were a last resort, and have, as a result of advances in lung surgery and tuberculosis-therapy, largely disappeared. One can imagine that these methods were especially “interventional”. The effectiveness was once upon a time described as good. In addition, our recent observations included no mention of any protest or opposition.
92. On account of general completeness, we would like to show the poor next patient.
Picture 92 : an unusual form of thorax calcification.
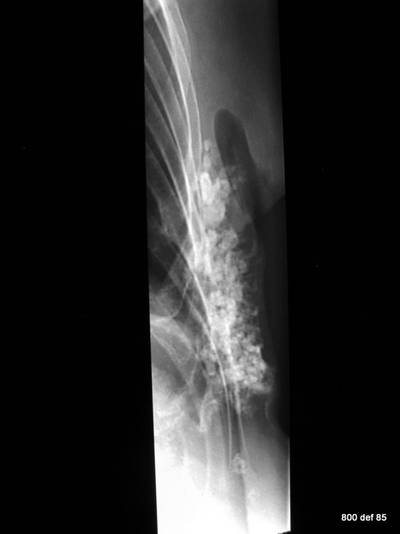
Where is it localised? What illness can the 72-year old lady have endured?
The question is not fair. Because, first and foremost we ought to question and examine the patient.
Medical condition: in strict accordance with “Ablatio mammae.” Condition after a secondary period of healing and infection of the thorax wall. Calcification in the thinned-out and scarred soft tissue area above the ribs: Calcification in a scarred plate area.——————
Picture 92b: A complication wich should not happen; Aspiration of BaSO4 7 years before
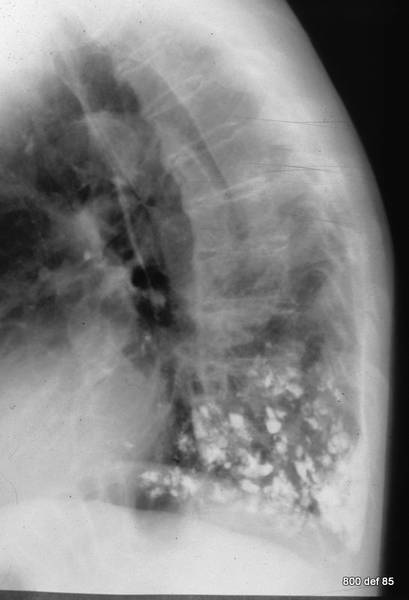
Cases 93-95; Pleural empyema
In the following text we are going to address two topics which enjoy more clinical significance (This is after the rare incidences of oleothorax)
– Pleural empyema (these alone, therefore, are so very important , because they do represent serious illnesses with a high letality rate) as well as …….
– Pleural differential diagnosis and pulmonary space demands.
Till now, we have concerned ourselves with only chronic empyemas. Our cases 40-75 were all almost those of empyema – at least in the widest sense. But there were organisational shapes, clinically silent, or indeed reactivated. The message was: these “Light classifications III” display a false sense of peace.
Now, let us turn to the acute shapes whwere is no doubt the patients are seriously ill; those of Light classification I and II .
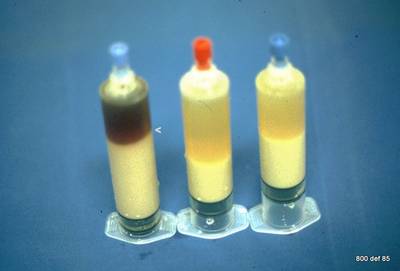
93. Three drained empyemata.
Downward sedimentation of the Leukozyten. Separation of of the cellular and interstitial components.
Picture 93: 3 results of pleural emyema aspiration. Notice the sedimentation of cells and the cell free exsudate. In rare cases an fatty degeneration of leucocytes results in floating cell material (here not shown).
How serious is pleural empyema? Is the treatment quite simple?
– Pleural empyemata are very serious and very grave illnesses (in certain situations and hospitals, the lethality rate is currently standing at 50%, but this should improve )
– The therapy is very difficult (complicated localisation results in a difficult possibility of full drainage).
These important remarks about Pleural empyema
represent the most serious statements in my paper. Patients lose their lives because doctor’s experiences are so widespread and the condition is so widely-underestimated.
Picture 94: Why does the localisation vary so strongly?
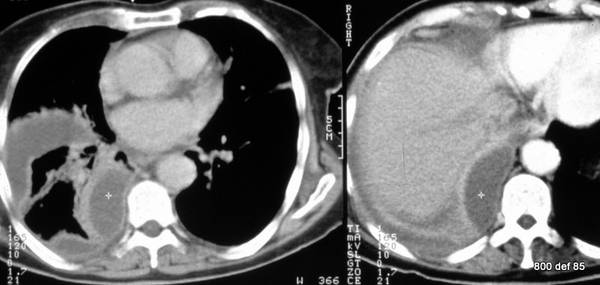
Why, for that reason, is the therapy so very difficult? Explain it on the basis of the case presented.
The localisation of the empyema is, due to the (already existing) pleural adhesions, especially multi-shaped. –
As to this patient, the empyema gathers itself in an “interlobar” fashion and in the dorsal paravertebral region. Without a CT or without an ultrasound, a sufficient point is quite hopeless. Even with the support of an image, it remains “art in the extreme.”
A single drainage is overwhelmingly insufficient. Even in a good state of a Drainage-value (from a larger diameter), it quite often transpires that, due to the tenacity and the coagulation aspect, the material enjoys no total aspiration at all.
It is necessary to form a surgical team with a committed and patient attitude. The surgeon enriches us with his experience in mini-thoracotomy and pleuroscopy. The radiologist performs the decisive elements during the translation of the images in the situation as concerns the “situs. I see no chance for either the radiologist or indeed for the surgeon.
95. In the past fortnight, the patient has suffered from a very serious lung infection. In spite of improved infiltrates in the lung parenchyma, there are still signs of more pronounced infection, more pronounced illness sensation with fever and tickling in the throat.
What differentiates the left from the right picture? The left slice is little more cranial than the right picture.
Picture 95: Enhancement of both pleurae? thin, fatty layer between the pleura parietalis and the thorax inner wall? Some air in the pus?
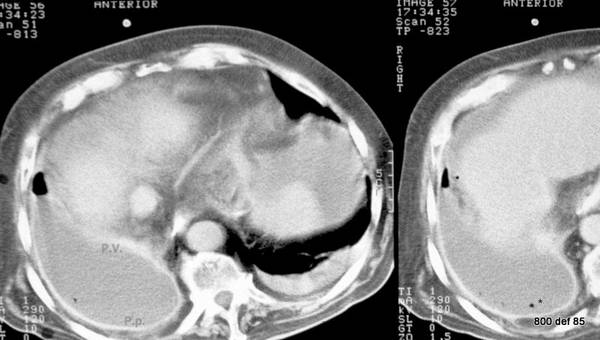
Diagnosis?
– The slice to the left lies in a more cranial manner
– Contrast is given intravenously. The decisive difference in effect: the left is significantly small, the right is sufficient.
– Diagnosis: pleural emyema following pneumonia.
– Enhancement of both pleurae.
– A thin, fatty layer between the pleura parietalis and the thorax inner wall. That means not a chronic process.
– The fact that this layer is only thin is an important sign for acute pleural empyema and permits a differentiation between chronic, persistent effusions with their wide fat strips.
(even the plombage , 76-92, have – generally- these thin, fat-rich layers. But history was compleatly different in this case)
– After diagnostic drainage, some air was to be found in the pus. This air gradually increased to the highest point of the caverns. Gradually the air, after 15 minutes, became ensnared in the pus. The tenacity of these suppurative materials proved this to be the case.
I maintain the following: the probe incision from 1 milliliter air (or 1 milligram CM) is especially informative about the possible or indeed impossible draining capability. It is, therefore, lawful, especially if one is classified or graded by many as useless and risky. The information bonus and benefit is colossal and quite possibly, life-saving.
From a sonographic aspect, quite often the impression of “septa” within the empyema can exist. We don’t know whether it may be a fact or an artefact. Anyway it reminds us to be avare of a difficult puncture.
Indisputable fact: air which is not distributed (i.e. “trapped air‘) as well as the sonographic impression of septa actually represent alarm signals for a very grave condition. A insufficient drainage is potentially inadequate.
Cases 96-100 complication of the empyema. What are typical discoveries in pleural empyema ?
Picture 96: To repeat the findings: further case of a voluminous pleural empyema. This time, on the left-hemithorax side.
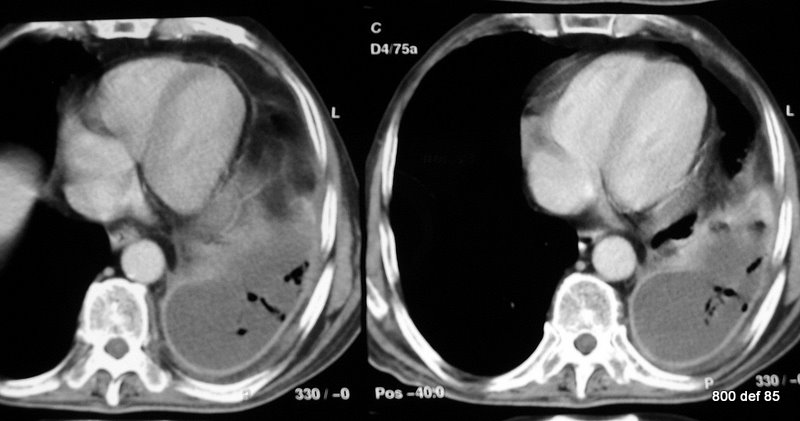
The air that has not ascended to the ventral, but is somewhere or other trapped air in the pus, represents a neglected sign for …
A difficult possibility for drainage that means a sign for bad prognosis. If the sign of alarm is well understood and will all facilities be activated, there remains a chance to control the situation.
97. However a significant accumulation of ‘pleura parietalis” has been the net result. The “pleura visceralis” has been tangentially sliced in the caudal sectors and , because of the subsequently resulting fuzziness of the edges, it is not easy to detect.
Picture 97: As concerns this particular patient, there is only a poor CM (contrast medium) presence
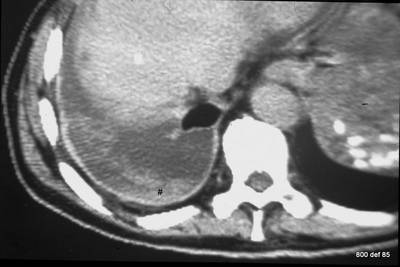
What, precisely, are the fluffy dense areas little#sign within the the empyema (in the pus location )?
Here we are talking about a build-up of the “cell-detritus”as regards the corresponding sedimentary Leukozytes. This material was, in all probability, partially shaken in the settling-down process of the patient, and then returned slowly to its lowest point.
Crucial: Homogeneity are not compulsory for structure of an acute, suppurating empyema.
98: Additional right-sided Pleural empyema
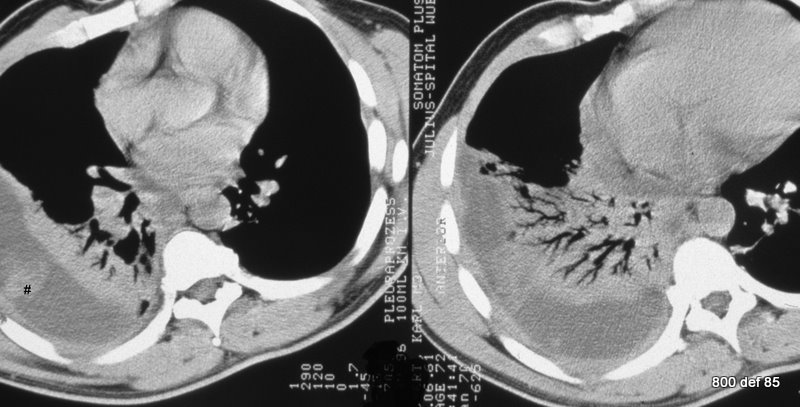
Was CM (contrast) employed at all? Are the changes of lungs a complication or an initial illness?
– Native series (no CM)
– Appropriately, the pleurae are less clearly restricted. Because of the significant space-demand of the empyema, an impressive “compression atelektasis” is to be found. This equates to a ventilation of the parenchyma. The bronchi, on the other hand, still contain air; because of their cartilage structure, they are less compressible and are liberated through the breathing movement and coughing-up of fluid.
– Without the detailed knowledge of the course, we are unable to decide whether it is only an “obturation atelektasis” or an infection of parenchyma is still present. In other words, compression atelektasis is present through a room-demanding empyema, or whether it is all about a remaining pneumonia, which became complicated through the empyema is present.
Picture 99: New case, administration of contrast (see the large vessels). Compression atelektasis
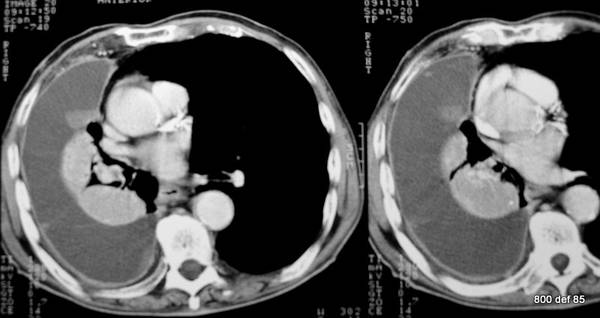
Does the atelektasis enhance CM? Does the “atelektasis” still contain air?
– The atelektasis in this case certainly contains still enough CM . One may assume that during the total airing, the blood circulation is restricted and checked in a reflectionary manner.–Thereby the enhancement will stop.
– The remainder ventilation is not so clearly-defined as per the previous case, but it is still in place.
(The greak word “ateles” means a type of meat, therefore “air-free” ; it is something of a paradox to speak of a “atelektasis” ; much better would be to speak about a “tendency to atelektasis.”)
In this and in the previous case, there was also this flecked density within the empyema area. This contained a conglomeration of pus cells.
Picture 100: A repeat: what are typical findings in pleural empyema ?
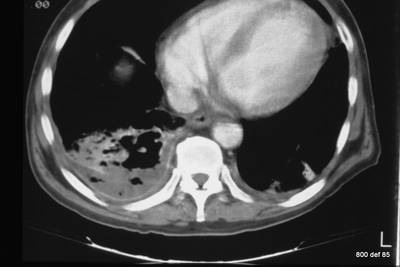
How many signs have you actually recognised in total?
– Localisation: multi-shaped, multi-sided ,so far rather untypical. To that end, the drainage is difficult or very diffucult.
– The empyema is often not homogenous because of irregular mixed cell-rich / protein-rich content.
– The tenacity of the empyema: thereby, a completely atypical distribution of trapped air content.
– One of the complications: the compression atelektasis with the corresponding subsequent infection threat of the lung-parenchyma.
Cases 101-105 highlights as concerns the differential diagnosis
101. A few highlights as concerns the differential diagnosis
within pleural/ pulmonal pathology.
Picture 101: The history clarifies the situation. Bronchial carcinoma as well as pneumectomy on the right side.


As far as this patient is concerned, there is no clinical treatment. There is no sign of septicemia which lends any evidence of empyema.
What precisely compensates the total volume loss of a lung? Can the individual components, which compensate for this volume loss, weigh in a different fashion?
Of note is
– the shift of the mediastinal to the right
– the hyperinflation of the left lung
– only a partially moderate deformity of the right Hemithorax
– within the remaining parietal pleura – only this pleural layer remained – a moderate serothorax.
The individual components, which compensate for the volume loss of a lung, can counter-balance this in different ways : this varies from case to case. The repair process, which attacks the volume loss with a similar mechanism, returns back again in varying ways to the compensatory possibilities.
New Patient. 102. Peel-thin, very regular wall calcification. From the other slices we know it is a sherical formation in mediastinum (a cyst).
Picture 102: 40 years old corresprondent for Asia.
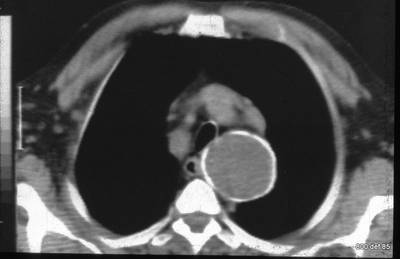
What is most conspicuous is the missing contour congruence of the thorax wall. The cyst clearly has nothing whatsoever to do with the pleura. A cause of suspicion towards an Echinokokkus cyst , due to the history, was declared.
103. This patient has been suffering for the past two months : illness sensation, dyspnoe and loss of weight. It is only at the very first glance that a similarity – morphologically-speaking – with empyema exists. The clinical tests, as well as the normal CRP value , do not address this as a pleural empyema.
Bild 103 : New patient; he is very ill; loss of weight
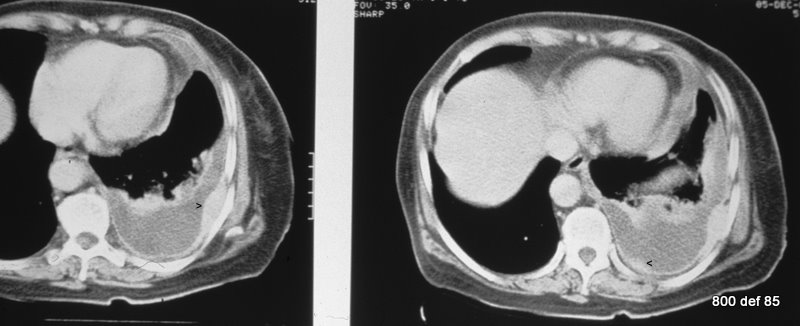
Also, what morphological discovery is “Empyem -atypical ?” Diagnosis? Suspicion?
The strong enhanced pleura is nodular-thickened in at least two areas. Thereby, a smaller perikardial effusion flowing with the thickening of the perikard leaves.
Urgent suspicion of carcinomatose pleurisy ( and also of carcinomatose perikarditis). Primary not known.
104. The carcinomatose pleurisy leads to no difficulties as concerns diagnosis : mutliple, irregular, knotty, gnarled thickening of the pleura, circumferential thickening ( more than 1 cm) and medistinal involvement. Quite often it is far more difficult. The cause of that particular CT-diagnosis enjoys a high specificity but, in contrast, a rather low sensitivity (Leung).
picture 104 : New patient. “Hypernephroma.” 4 years ago
What could be the possible reason for such a carcinomatose pleurisy?
Bronchogenic carcinoma, lymphoma, breast carcinoma, metastatic spread arising from abdominal tumours. The precise relative frequency are not known to me.
105. To continue with neoplasms
picture 105

The diagnosis is much easier since intravenous contrast had been administered. The patient displays a – small, fresh pleural effusion on the right, which has subsided in a supine position towards the dorsal area,- as well as a loculated effusion on the right, aside the ventral side.
But what is the main diagnosis?
On the right and centrally-located: broncial carcinoma ;
The neoplasm probably grows in the larger veins (that flow towards the left atrium). – Such a tumour can infiltrate the pleura or grow in a metastasic way. The most secure clinical sign for infiltration is pain.
Cases 106-110 oncology, heterotopic thyroid, teratoma
Picture 106: A patient from oncology (Hypernephroma). Thirty years ago, this particular patient suffered from tuberculosis.
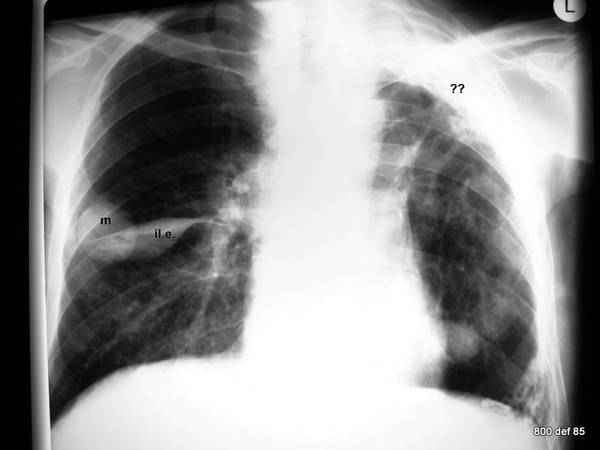
What are the various findings? What may be confirmed?
– Two significantly large coin lesions ( in the right to mid region as well as in the left lower part)
– a “spindle-shaped” shadowing on the right: this signifies an interlobar effusion.
– Wide pleural shadowing in the left apex area.
But what we are unable to detect here is as follows : as an exception to our objective less under-exposed radiographs and one which contains sufficiently high KV, shows the calcification of both pleurae. In effect, therefore, a remnant empyema after an old tuberculosis.
Furthermore, there was evidence of calcification in the area of the pleura diaphragmatica.
In addition, signs of lung adhesions, which condense and lift the left hilus towards the top.
In summary tis poor man suffered from a combination of a metasatic Hypernephroma together with an old tuberculosis.
107. 55 years old lady. Euthyreosis.
Thoracic space-occupying lesion during a course of at least 12 years. This contains calcifications.
Picture 107 : Hardly any feeling of sickness; only mild stridor. No signs at all of any infection.
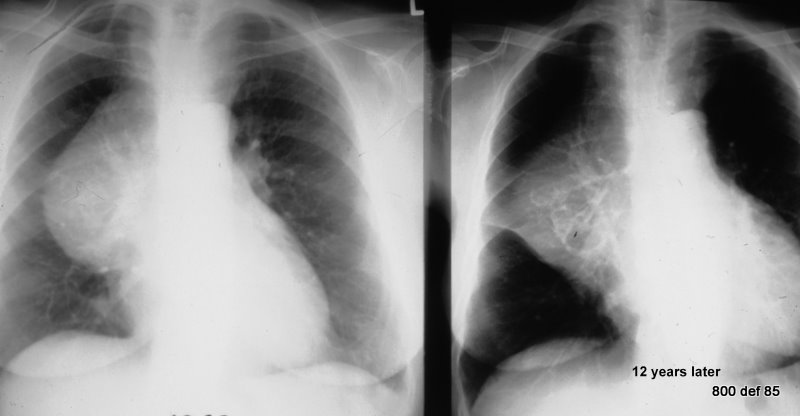
There are 12 years between the two images. This follow-up is helpful for diagnosis.
The very minor change during the 12-year course of events speaks against a malignant tumour as well as against lymphoma.
It might suggest a Struma or a Teratoma.
Would nuclear medicine be of use ?
108. The same patient: Remarkable and obvious storage of Nuclid within the tumour. (szintigraphy is interrupted, thereby the linear limitation below ).
This Thyroidea-szintigraphy with TcO4 and Thorax-X-ray are duply projected one on top of the other. The use of TcO4 ism’t sate of the art.
Picture 108: We are dealing with a large heterotopic thyroid part.
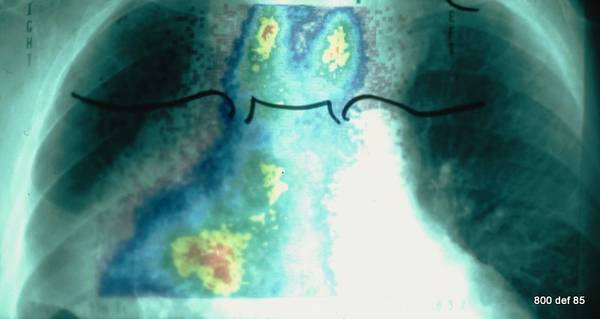
Diagnosis?
It is not skilfull and arty to perform such a retrosternal struma with TCO4, because there are better tracers for this geometric and biological situation.
But the result is sufficient.
Finaly remember the 4 x T for mediastinal masses:
- Thyreoidea
- Tymoma
- Terratoma (see next case)
- Sir Thomas Hodgkin (Lymphoma)
Picture 109 : A 32-years-old patient with partially solid, partially fatty, partially calcified tumour in the the mediastinum (left). This leads to a distinct lung-compression and to storage of the hilus structure.
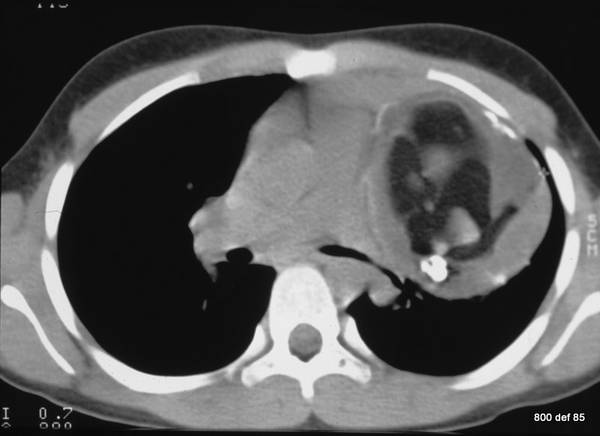
Little pain for about 4 weeks. So, a diagnosis?
A Teratoma (malformation tumor): this contains, typically, various tissues.
Picture 110: Another patient with a blotchy, speckled calcified tumor in proiection of the apex of the lung.
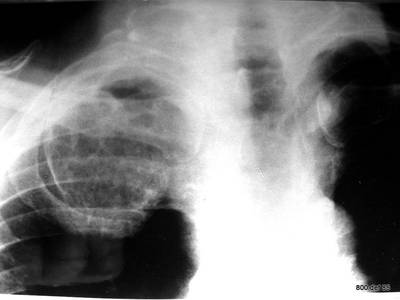
Accidental finding. No palpable mass. Likely diagnosis?
Rib number 1 cannot be distinguished. It appears as if it has caused a tumor. Enchondroma of rib number 1 is the likely diagnosis
and a benign tumor.
If in doubt, fluoroscopy or computed tomography would be of great help.
Cases 111-113 Asbestosis, pleural Mesothelioma, Silicosis
111. This woman patient had herself never worked with asbestos but merely ( over 7 years) cleaned the clothing of those people who had worked with asbestos.
Picture 111 : ” Pleural plaques.”
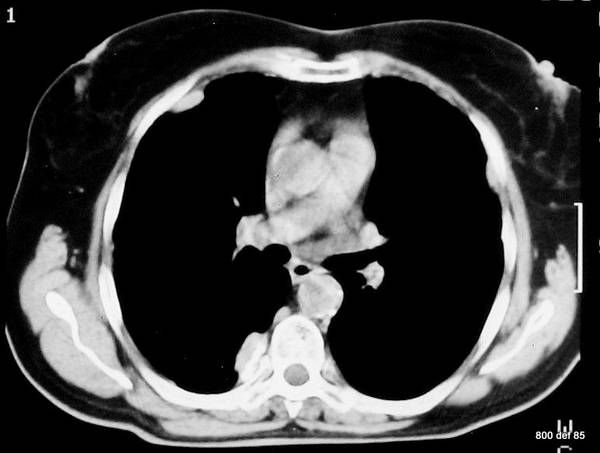
Here, on the right-hand side, at the paravertebral area, a calcification is discernible. Possible diagnosis?
This anamnesis is very suspicious. A pleural lavage will be carried out.
Together with the morphological findings (and positive pleural lavage!) : asbestosis.
As a result of the pleural reaction to asbestos, one may distinguish the following factors :
– the diffuse thickening of the pleura (decades-long underestimation in radiology : dismissed as totally banal rind-type thickening ;
only acknowledged by the pathologists as well as
– “pleural plaques” ( for details, see Otto ; Jend; Hering);
The latter so-called hyaline plaques are typical in both their elongation and thickness as well as in accordance with the closing of their exposition .
They cannot be detected before the fifth year of the exposition start and they further calcify after a subsequent five years. This calcification affects the parietal surface rather than the complete thickness of the plaques, which contains parts from both of the pleural sheets.
Picture 112 : This new patient has pleural plaques 20 years after being exposed to asbestos (did lot of work with heating pipes insulation).
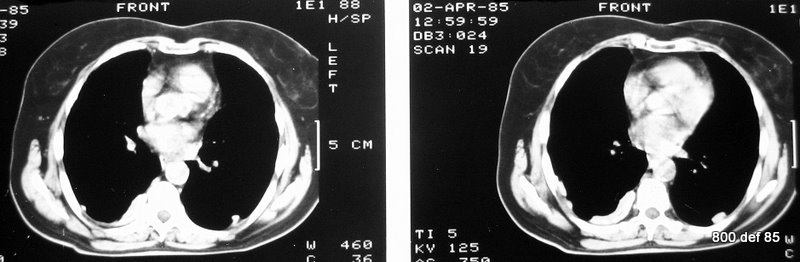
– Builders, carpenters, electricians; Die Wahrscheinlich
– Between 5-10%;
– Das Maximum der Mesotheliome wird im Jahre 2017 erwartet ! Wenn die Prognose gestimmt hat, haben wir die schlimmste Phase hinter uns. Trotzdem wird es weiter Mesotheliom- Fälle bei Asbestosen geben. Leider gibt es auch Neuinfektionen bei den weltweiten unsachgemößen Abbrucharbeiten von verseuchten Bauten.
Das maligne Pleuramesotheliom: Dtsch Arztebl 2000; 97(48): A-3257 / B-2739 / C-2426 ; ; ; ; ;
Picture 113 : New patient. Condition with known asbestos exposure
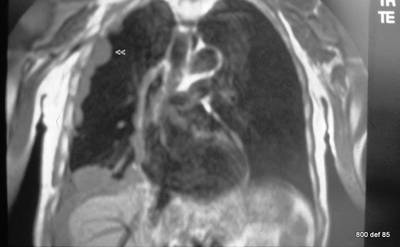
MR in coronar projection. The right lung cased entirely around by “foreign” tissue structures. Possible diagnosis?
Pleural Mesothelioma ( for details, see the literature)
Cases 114 – 120 Silicosis; and a repetition of the many signs of fibrothorax
As radiologists from many areas of Europe, we are, as regards this particular thorax film quite helpless. But, in some areas and some hospitals,
one recognizes this conditions very well indeed.
Picture 114: New patient with many findings on his chest x-ray. We are lucky he can tell us more about his work and his medical history
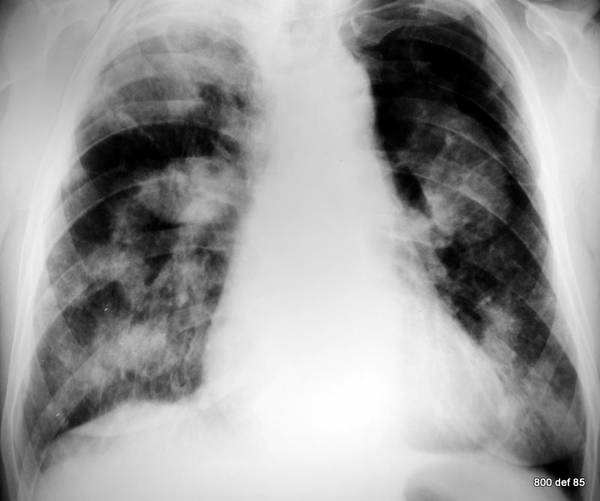
So, what does one ask the patienth having wich Diagnosis in mind?
Occupational disease? Exposure? Duration of exposure? –
Diagnosis: Silicosis.
This case involves a miner who toiled at the rock face for 15 years. The way in which miners have been exposed, has been well recorded and documented : quite often a professional disease has already been acknowledged. The clinical condition of the patient was remarkable good. However we are glad those boys are much less exposed in our days.
Picture 115 : An other miner; case study as regards the “multi-faceted findings behind silicosis”
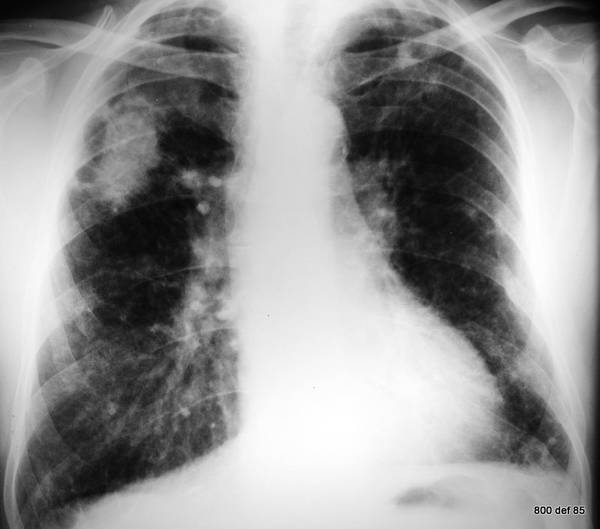
As well as the
– silicotic homogeneously consolidated areas in the right upper region. In this country they call the closely packed shadows “Ballungsherde”. There also exist
– pleural thickening and
– multiple mid-to-finely flecked opacities in the periphery of the lungs.
The radiologist, who – just as I – is not trained in the study of pneumokoniosis, should not attempt to carry out a medical assessment. He should,
however, be able to reach a basic conclusion. One must know where one may be able to access a competent and definitive reference work.
3 more cases without discussion:
Picture 116 : Silicotic “packed shadow” in the CT. The functional impairment can be minor.
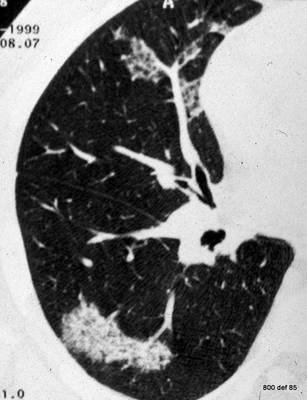
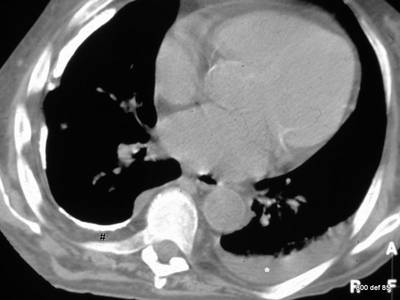
Repeat again: What precisely are those findings? What acute occurrence probably took place on the right-hand side?
– Thick, coarse and calcified fibrothorax on the right-hand side and
– shrinkage of the thorax caverns.
– Thickening of the ribs (see Eyler et al.).
– A partially uncalcified layer between the pleura and the ribs
– however, no distortion of the heart or mediastinum towards the right side.
– On the left side, a fresh pleural effusion, possibly linked to the clearly enlarged heart.
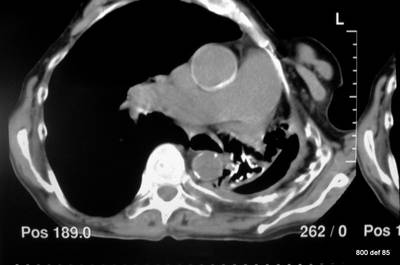
Picture 118: Massive distortion of the heart area and of the mediastinum on the left side, dilatation of the pulmonary arthery.
What happens with the pleurae? Were this tension comes from?
To be found: a chronic Empyema on the left side with scarred deformity, bronchiectasis in the shrunken left lung, massive distortion of the heart area and of the mediastinum on the left side, dilatation of the pulmonary artery under tension of pleural scar.
What acute occurrence most probably took place on the right-hand side?
(Click here for the answer)
Bronchopleural fistula, connection to and with the pleural space; contents of empyema entirely drained via bronchial system. Thereby, the filling-up of the empty space with air. That is what we found in case 76 too; so, we come back to the start of this article.
Propably a chronic empyema is the reasen for all the findings. It conected with the prnchial system and the content is cought out und the cacity is filled with air. dilatation of the pulmonary arthery under tension of pleural scar.
Ask me what exactly is the “Crux of the Pleura” ?”
One hardly detects the normal pleura.
One can only see it in the pathological sense and then there is not the professionalism to be able to distinguish between what pleurae are and what may lie in between. That was my main topic, my main theme. In special cases, ( e.g. Calcification) everything is much simpler, provided that, of course, one seizes this
unbelievable assistance of Nature itself. Calcification is the large didactic chance for all of us: this is what H.G. Schmitt has formulated. He has battled
against the myth ( or is it only a weak and a poor excuse !), namely that the contents of the pleura-caverns are “fibrous tissue”. Such a case was never proved. (The proof and the evidence will at least lend itself to a most clear enhancement of intravenous contrast.)
The MR is rarely necessary : if it is , however, conducted, then it will be didactically beneficial.
picture 119 : Another chronical empyema; the puncture picture on the right; the fluid is aspirated on the left pic., air in the cacity